This aspiration echoes widely across modern society. As global life expectancies continue to rise, individuals are increasingly focused not only on living longer but on maximizing their "healthspan"—the period of life spent in good health, free from chronic disease and disability. The allure of remaining fit, lean, and youthful into advanced age, perhaps even reaching 90, 100, or beyond, is undeniably compelling. However, the prevailing narrative surrounding health and longevity often suggests an extraordinary commitment of time, effort, and financial resources, leading many to question its feasibility and ultimate efficacy.
The Evolving Landscape of Longevity Advice
The pursuit of a longer, healthier life has captivated humanity for millennia, from ancient remedies to modern medical breakthroughs. Historically, significant gains in lifespan were primarily driven by improvements in public health, sanitation, nutrition, and infectious disease control. In recent decades, medical science has further extended human life through advancements in treating chronic conditions like heart disease and cancer.

More recently, a new wave of "longevity optimization" has emerged, propelled by influential figures in health and biohacking. Podcasts, books, and social media platforms are awash with intricate protocols, cutting-edge supplements, and advanced diagnostic tests championed by experts such as Dr. Peter Attia, Dr. Andrew Huberman, Dr. Rhonda Patrick, and biohacker Bryan Johnson. This movement promises to unlock unprecedented levels of health and extend life far beyond average expectancies, offering a comforting sense of control over one’s biological destiny.
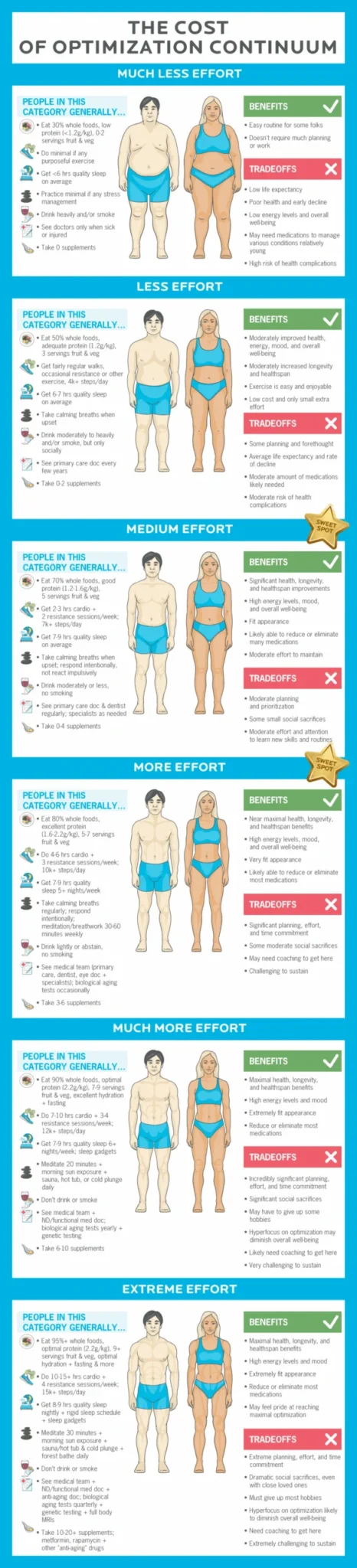
Yet, this surge of complex advice has created a dichotomy. While the desire for optimal health is universal, the practicality of implementing these high-effort, high-cost strategies remains a significant barrier for most. For organizations like Precision Nutrition, with extensive experience coaching hundreds of thousands of individuals through real-life challenges, the concept of "optimal" often clashes with "realistic." Their collective insight suggests that true, sustainable health gains are rarely found at the extreme end of the optimization spectrum.
Deconstructing the Myths of Hyper-Optimization
The prevailing culture of longevity optimization often perpetuates several myths that can deter individuals from pursuing effective, sustainable health practices.

Myth 1: The "Basics" Aren’t Enough for Significant Longevity
A common misconception is that achieving exceptional health and outliving average expectancies necessitates a suite of complex, "cutting-edge" strategies. This belief dismisses the profound impact of fundamental health behaviors. In reality, consistent adherence to basic principles—regular exercise, a nutrient-rich diet, adequate sleep, stress management, and social connection—yields remarkably powerful results.
The critical issue is not the insufficiency of these basics, but the widespread inconsistency in their application. For instance, according to the Centers for Disease Control and Prevention (CDC), only about 24% of U.S. adults meet the recommendations for both aerobic and muscle-strengthening activities. Similarly, less than 10% of Americans consume the recommended five servings of fruits and vegetables daily. The gap in longevity and health isn’t primarily due to a lack of ice baths or vitamin infusions, but rather a failure to consistently implement these relatively simple, proven practices. Individuals who consistently engage in a well-rounded set of health-promoting behaviors at an 80-90% consistency rate are often already near their peak health potential.
Myth 2: More Effort Always Equates to Better Results
The intuitive appeal of "more is better" often leads individuals to believe that perfectly executing and maximizing every health behavior will inevitably lead to superior outcomes. However, health and fitness efforts are subject to the law of diminishing returns. Initial efforts in areas like exercise or diet often yield substantial improvements, but as these efforts become more extreme, the additional benefits become increasingly marginal.

Beyond a certain point, excessive commitment to a health regimen can introduce counterproductive elements. It can lead to burnout, increased stress, social isolation, and financial strain. The purpose of extending life and healthspan is to live a full, enjoyable existence. If the pursuit of "more" detracts from overall quality of life, the fundamental objective is undermined. For example, overtraining can disrupt hormonal balance, impair sleep, and increase injury risk, negating many of the benefits of exercise.
Myth 3: Cutting-Edge Strategies Offer Guaranteed Significant Benefits
Many advanced, complex longevity strategies touted by influencers and biohackers lack robust scientific validation. Much of the research supporting these fringe methods is often preclinical (conducted in mice or cell cultures), observational, theoretical, or tested on very small cohorts for short durations. For example, popular supplements like NAD+ precursors or resveratrol show promise in animal models but have limited, if any, conclusive evidence of significant longevity benefits in humans.
Furthermore, some of these unproven methods and supplements can be potentially unsafe. The unregulated nature of the supplement industry means products may contain unlisted ingredients, incorrect dosages, or contaminants. Prioritizing foundational, evidence-backed health behaviors offers a far more reliable and safer pathway to improved health outcomes than investing in speculative, unproven interventions.

Myth 4: It’s An All-or-Nothing Endeavor
The perceived monumental effort required for "optimal" health can overwhelm individuals, leading to inaction. The belief that one must adhere to a perfect regimen (e.g., waking at 5 a.m. for 90-minute runs to optimize VO2 max) or risk failing entirely is a significant barrier.
However, data from long-term coaching programs demonstrates that even modest, inconsistent efforts can yield measurable results. For instance, clients in year-long coaching programs who practiced basic habits less than half the time still achieved significant improvements in body composition and overall health markers. This underscores that progress is incremental and accessible. Health is a continuum, not a binary state. Small, consistent improvements, even when imperfect, accumulate over time to create substantial positive change. It is crucial to dispel the notion that great health is beyond the capabilities of those unwilling or unable to commit to extreme optimization.
The Foundational Pillars of Health and Longevity
True health and longevity are built upon a bedrock of consistent, fundamental behaviors that are scientifically proven to reduce disease risk and enhance quality of life.

1. Exercise Regularly: The Cornerstone of Physical Vitality
Physical activity is unequivocally one of the most powerful tools for extending both healthspan and lifespan. Research consistently demonstrates that any amount of physical activity significantly reduces the risk of all-cause mortality, independent of other lifestyle factors like diet or smoking habits. A seminal study of Harvard alumni, for example, highlighted the universal benefits of exercise in extending life.
Specific benefits include improved cardiovascular health, enhanced mood and cognitive function, better energy levels, and increased functional independence in older age. Exercise also plays a critical role in mitigating the risk of chronic diseases such as type 2 diabetes, certain cancers (e.g., breast, colon, colorectal), and osteoporosis.
Optimal Dose: Standard guidelines from organizations like the World Health Organization (WHO) and the American Heart Association (AHA) recommend:

- Aerobic Activity: At least 150-300 minutes per week of moderate-intensity aerobic exercise (e.g., brisk walking, cycling) or 75-150 minutes of vigorous-intensity aerobic activity (e.g., running, swimming laps), or an equivalent combination.
- Resistance Training: At least two days per week of moderate-to-high intensity muscle-strengthening activities involving all major muscle groups.
Accumulating 7.5 to 15 MET-hours (Metabolic Equivalent Hours) of activity per week is associated with significant risk reduction, with further benefits plateauing thereafter. Even small increases in daily steps—as little as 1,000 steps—are linked to a 12% lower risk of death, extending up to 17,000 steps. For cognitive health, studies show that just 3,826 steps per day can reduce dementia risk by 25%, with 9,826 steps lowering it by 50%.
Risks of Overtraining: While more exercise is generally better up to a point, extreme volumes of endurance training (e.g., ultra-marathons) may carry risks such as myocardial fibrosis, coronary artery calcification, and atrial fibrillation, illustrating the "Extreme Exercise Hypothesis" where both very low and extremely high activity levels are associated with increased health risks.
2. Eat a Nourishing, Nutrient-Rich Diet: Fueling Longevity
A healthy diet doesn’t require extreme restrictions or exotic ingredients. It centers on a few key nutritional fundamentals.

Nutritional Key 1: Prioritize Whole and Minimally-Processed Foods. These foods are naturally rich in fiber, healthy fats, vitamins, minerals, and phytochemicals, while being less calorie-dense and containing fewer added sugars, sodium, and unhealthy trans fats than highly- or ultra-processed foods (UPFs). Diets rich in whole foods are linked to lower rates of depression, heart disease, type 2 diabetes, and cancer, and improved longevity. Conversely, a comprehensive review of nearly 10 million participants found UPFs linked to 32 harmful effects, including obesity, cardiovascular disease, and all-cause mortality. Individuals who consume four or more servings of UPFs daily face a 62% increased risk of all-cause mortality, with each additional serving increasing risk by 18%.
Optimal Dose: Aim for 70-80% of your diet from whole or minimally-processed foods. Even reaching 50% can yield substantial benefits. Beyond 90%, additional benefits are likely negligible, and some processed foods (e.g., protein powder) can be health-enhancing.
Nutritional Key 2: Consume Five Servings of Fruits and Vegetables Daily. A meta-analysis of over 1.8 million people found that five servings of fruits and vegetables daily reduced all-cause mortality risk by 13% compared to two servings. These foods are packed with diverse phytochemicals, each offering unique health benefits.

Optimal Dose: A target of five fist-sized servings daily (three vegetables, two fruits) is ideal, focusing on a variety of colors. Benefits tend to plateau at this intake, meaning more than five servings doesn’t necessarily confer additional life-extending advantages.
Nutritional Key 3: Ensure Adequate Protein Intake. Protein is crucial for muscle maintenance, especially as we age, combating sarcopenia (muscle loss), frailty, and neuromuscular decline. It supports bone health, immunity, and satiety. Plant proteins are particularly linked to reduced cardiovascular disease and all-cause mortality. While animal proteins offer benefits, processed red meats should be limited, and unprocessed red meat to about 18 oz per week.
Optimal Dose: The current USDA minimum is 0.8 g/kg body weight, but a better minimum for most, especially older adults, is 1.2 g/kg (0.55 g/lb). For muscle growth, recovery from vigorous exercise, or individuals on GLP-1 medications (which can cause muscle loss), 1.6-2.2 g/kg (0.75-1 g/lb) is optimal.

3. Get Adequate Sleep: The Foundation of Recovery
Sleep is a non-negotiable pillar of health. Studies show that men getting sufficient quality sleep live almost five years longer, and women two and a half years longer. Sleep is as vital for heart health as exercise and diet. A one-hour decrease from 7 hours of sleep is linked to an 11% increased risk of cardiovascular disease and a 9% increased risk of type 2 diabetes. For older adults, less than 6 hours of sleep increases the risk of dementia and cognitive decline, as deep sleep is crucial for clearing brain toxins.
Optimal Dose: 7 to 9 hours of quality sleep per night is ideal for most adults. The "right" amount is when you feel refreshed upon waking and maintain sustained energy throughout the day.
Risks of Excessive Sleep: While not as clearly causal, consistently sleeping over 9 hours per night is associated with increased risks of cardiovascular disease, type 2 diabetes, and overall mortality. This may indicate underlying health issues (e.g., depression, sleep apnea) rather than sleep itself being harmful.

4. Manage Stress: Building Resilience
Chronic, unmanaged stress profoundly impacts nearly every physiological system, increasing heart rate, blood pressure, and inflammation, thereby elevating the risk of cardiovascular disease. It also worsens mental health, contributing to anxiety and depression. However, stress is a natural and even beneficial part of life; the right amount can motivate and engage us.
Effective Management: Stress management isn’t just meditation. It encompasses self-compassion, a growth mindset, and framing stress as a normal part of life. Developing self-regulation skills—noticing emotions, controlling reactions, and employing diverse coping mechanisms—builds resilience. Practices like deep breathing, journaling, gentle stretching, or spending a few minutes outdoors can significantly replenish one’s "recovery jug."
Optimal Dose: Stress management should be proportionate to life’s demands. Three to five minutes of purposeful recovery can make a difference. The goal is to find a "sweet spot" where you feel energized and engaged, rather than bored or overwhelmed. Over-scheduling stress reduction techniques can paradoxically add more stress.

5. Stay Socially Connected: The Human Imperative
Social connection is a powerful determinant of health and longevity. Strong social and emotional support is linked to improved well-being and a 50% increased likelihood of survival. The Harvard Study of Adult Development, spanning over 87 years, identified strong relationships as the biggest predictor of life satisfaction and longevity, even surpassing social class, wealth, IQ, or genetics.
Conversely, social isolation and loneliness significantly increase risks for heart disease, stroke, type 2 diabetes, depression, anxiety, dementia, and premature death. The mortality risk associated with social isolation is comparable to smoking 15 cigarettes a day, exceeding risks from obesity or physical inactivity.
Optimal Dose: Research suggests that having three to five close friends with whom one interacts regularly (1-3 times per week, in-person or by phone) provides the most social benefit. Quality over quantity is key; a smaller, authentic network often yields more benefit than a large network of acquaintances.

Risks of Excessive Socialization: Some evidence suggests excessive daily social engagement might slightly increase mortality risk, potentially due to increased fatigue, exposure to unhealthy behaviors (e.g., heavy alcohol use), or diverting time from other health-promoting activities.
6. Minimize Known Harms: Protecting Your Future Self
Actively avoiding or minimizing known harmful activities is a fundamental aspect of long-term health, though often overlooked due to personal preferences. The two most significant culprits are smoking and excessive alcohol consumption.
Harm Avoidance 1: Don’t Smoke. Tobacco use remains a leading cause of premature death globally, accounting for over 8 million deaths annually. It is a major risk factor for coronary heart disease, stroke, emphysema, and numerous cancers, contributing to about a quarter of all cancer deaths worldwide. Despite widespread awareness, smoking still affects a significant portion of the population, including 11.5% of adults in the U.S. and 15% globally. The message is unequivocal: complete abstinence from tobacco is paramount for longevity.

Harm Avoidance 2: Limit Alcohol. The scientific consensus is increasingly clear: alcohol has negative implications for health, particularly with regular, heavy use. It plays a causal role in over 200 diseases, including liver diseases, heart conditions, at least seven types of cancer, depression, anxiety, and dementia. In 2019, alcohol was responsible for 2.6 million deaths globally, and for individuals aged 15-49, it is the leading risk factor for death.
Optimal Dose: U.S. guidelines recommend moderate intake: up to one drink per day for women and up to two drinks per day for men. A "drink" is defined as 14 grams of pure ethanol (e.g., 12 oz beer, 5 oz wine, 1.5 oz spirits). The WHO’s 2023 statement suggests no amount of alcohol is "safe," but this interpretation is debated. While small doses may have negligible health impacts, risks rise exponentially with heavier drinking (more than 3-4 drinks on a single occasion or more than 7-14 drinks per week). The goal is informed decision-making based on individual risk tolerance and overall life priorities.
7. Basic Preventive Health Measures: The Unsung Heroes
Beyond daily habits, consistent engagement in basic preventive health measures is crucial. These "boring" but vital actions include:

- Regular medical check-ups and screenings (blood pressure, cholesterol, cancer screenings).
- Vaccinations (flu, COVID-19, shingles, tetanus).
- Dental hygiene (brushing, flossing, regular dental visits).
- Vision and hearing tests.
- Safe practices (wearing seatbelts, helmets, sunscreen, hearing protection).
- Maintaining a safe home environment (smoke detectors, fall prevention).
These measures are often overlooked in the quest for optimization but provide immense protection against preventable illness, injury, and early mortality. For example, hearing loss is the number one modifiable risk factor for dementia, emphasizing the importance of protecting auditory health. While many preventative measures are widely adopted (e.g., seatbelt usage at 92%), others like daily flossing (32%) or helmet use among cyclists (around 50%) show significant room for improvement.
It’s also critical to acknowledge social determinants of health—systemic factors like poverty, racism, and lack of access to healthcare—that make these protective behaviors harder, or even impossible, for many. The pragmatic approach is to "do the best you can with what you’ve got."
The Hidden Costs and Tradeoffs of Hyper-Optimization
While the foundational health behaviors offer substantial returns on investment, the pursuit of "hyper-optimization" comes with significant, often unacknowledged, costs and tradeoffs.

Time and Financial Investment: An "optimizer" lifestyle can demand three to four times the time, effort, and financial resources compared to a conventionally "healthy" lifestyle. Beyond the daily regimen of specialized diets, intense workouts, and meticulous tracking, optimizers often invest in less frequent but costly interventions:
- Advanced diagnostic tests (e.g., whole-body MRIs, genetic sequencing, extensive blood panels).
- Specialized therapies (e.g., cryotherapy, hyperbaric oxygen therapy, IV drips).
- High-end supplements (e.g., bespoke nootropics, peptides).
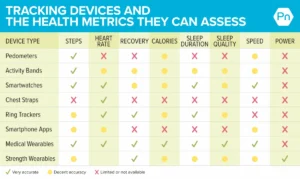
- Biofeedback devices and wearables (e.g., continuous glucose monitors, advanced sleep trackers).
- Personalized coaching and concierge medical services.
These expenditures can easily add tens of thousands of dollars annually, diverting resources that could be used for education, experiences, or financial security, which also contribute to overall well-being and a fulfilling life.
Impact on Well-being and Quality of Life: The relentless pursuit of "optimal" health can paradoxically undermine overall well-being. Excessive focus on physical health can lead to neglect of other crucial "deep health" domains: relational, existential, mental, and emotional health. An obsessive adherence to strict protocols can foster social isolation, rigid thinking, and even manifest as mental health conditions like orthorexia—an unhealthy obsession with healthy eating—or exercise addiction.

The "law of diminishing returns" applies not only to physical benefits but also to life satisfaction. While initial health efforts significantly boost well-being, hyper-optimization can plateau or even decrease it, creating a constant state of vigilance and self-deprivation. The essence of a long life should be to enjoy it. If the journey to longevity becomes a joyless, all-consuming endeavor, the ultimate purpose is lost. Enjoying life is not separate from good health; it is an intrinsic part of it.
Making Informed Choices for Your Health Journey
Navigating the vast landscape of health advice requires clarity, self-awareness, and a realistic perspective.
- Clarify Your Goals: Begin by reflecting on what truly matters most. What kind of life do you envision for yourself? How important is maximizing healthspan and lifespan relative to other life priorities like relationships, career, personal growth, or leisure?
- Consider the Tradeoffs: Honestly assess your available resources—time, money, and energy. How much are you willing to invest in health goals, and what are you prepared to sacrifice? Understanding these tradeoffs allows for intentional choices aligned with your values.
- Prioritize the Basics: Review the foundational health behaviors outlined in this article. Identify areas where you are consistently performing well and those that offer room for improvement. For the vast majority, focusing on consistent, moderate improvements in these core areas will yield significant, tangible results without the burdens of hyper-optimization. Embrace progress, not perfection.
- Tune Out the Noise: The cacophony of health advice from podcasts and social media can be overwhelming. Remember that these "experts" are not experts on your unique life, circumstances, or priorities. Empower yourself to make decisions that resonate with your personal values and goals. Your health journey is yours alone to define.
Ultimately, a truly healthy and long life is not about chasing every marginal gain or adhering to extreme protocols. It’s about cultivating sustainable habits, fostering resilience, and finding joy in the everyday, knowing that reasonable, consistent efforts are the most powerful investments in your long-term well-being.