This stark revelation emerges from a comprehensive study involving nearly 2,000 individuals grappling with Irritable Bowel Syndrome (IBS). The finding underscores the profound and often debilitating impact this chronic gastrointestinal disorder has on patients’ lives, pushing many to contemplate extreme sacrifices for relief. Further research has echoed this desperation, with some IBS sufferers expressing willingness to take a medication carrying a one percent risk of sudden death if it promised a complete cessation of their symptoms. These symptoms are far from trivial, encompassing urgent bouts of diarrhea, persistent constipation, excessive gas, and abdominal pain often described as more severe than childbirth.
The Debilitating Reality of IBS: Beyond Physical Symptoms
The daily reality for many with IBS is one of constant apprehension and careful planning. Flare-ups are unpredictable and can be devastating, draining concentration, disrupting sleep, and severely hampering work productivity. This pervasive fear often dictates social interactions and daily routines, leading individuals to meticulously plan their lives around the availability of clean, private bathrooms. Public activities, such as dining out, social gatherings, or even exercising, are frequently avoided due to the overwhelming anxiety of an unexpected symptom onset.
This profound worry has been formally recognized as gastrointestinal-specific anxiety. It infiltrates nearly every aspect of an individual’s life, from the integrity of their social relationships to their overall sense of well-being. This anxiety is a primary driver behind the reported lower quality of life among IBS patients compared to those with other severe chronic conditions, including heart disease, diabetes, and even end-stage kidney disease. The psychological burden of IBS is, therefore, as significant as its physical manifestations, creating a vicious cycle where stress exacerbates symptoms, and symptoms amplify stress.
Understanding IBS: A Functional Neuro-Gastrointestinal Disorder
Often colloquially referred to as "spastic colon," IBS stands as the most commonly diagnosed digestive disorder globally, affecting approximately 14 percent of adults. Despite its widespread prevalence, IBS has historically been misunderstood. Unlike inflammatory bowel diseases (IBD) such as Crohn’s disease or ulcerative colitis, IBS does not involve visible structural changes or damage to the gut architecture. Diagnostic imaging, endoscopy, and biopsies typically reveal no infections, inflammation, or physical lesions, leading many healthcare professionals in the past to erroneously conclude that the condition was purely psychological.
However, modern medical understanding has profoundly shifted. Experts now classify IBS as a functional neuro-gastrointestinal disorder. This definition highlights a critical dysfunction in the communication pathways between the gastrointestinal tract and the brain. In individuals with IBS, these nerves do not operate optimally, resulting in the brain misinterpreting normal digestive processes as pain signals and interfering with typical bowel functions. This altered gut-brain axis is central to the diverse and often perplexing array of symptoms experienced by patients.
IBS symptoms are highly variable and episodic, with individuals experiencing periods of relief lasting months or even years, only to be struck by severe flare-ups that can persist for hours or weeks. The lack of a uniform symptom presentation further complicates diagnosis. Common symptoms include abdominal pain, cramping, stool irregularities (ranging from chronic constipation to recurrent diarrhea, or an alternating pattern of both), excessive gas and bloating, the presence of mucus in stools, and a sensation of incomplete bowel movements.
Exploring the Etiology of IBS: Current Theories
While the precise mechanisms underlying IBS are still under active investigation, several prominent theories attempt to explain the altered gut function. One leading hypothesis centers on the idea of hypersensitive nerve endings within the GI tract. This heightened sensitivity means that normal digestive processes, such as the movement of tiny gas bubbles or minor muscle contractions, which would go unnoticed by individuals without IBS, register as intense discomfort or pain for those with the condition.

This oversensitivity can manifest in two distinct ways:
- Exaggerated Pain Signals: Hypersensitive nerves send amplified pain signals to the brain, leading to a disproportionate perception of discomfort from routine digestive activity.
- Dysregulated Muscle Contractions: Overreactive GI muscles may contract with excessive force, accelerating the passage of food and contributing to gas, bloating, and diarrhea (IBS-D). Conversely, if these muscles underreact, food transit slows significantly, leading to constipation (IBS-C).
Another compelling theory implicates disturbances in the gut microbiome, the complex community of microorganisms residing in the digestive tract. Research suggests that an imbalance or alteration in gut bacteria composition may play a crucial role in IBS development. This theory helps explain why some individuals develop IBS symptoms following a severe gastrointestinal infection, such as Norovirus, a phenomenon known as post-infectious IBS. The infection may trigger lasting changes in the gut microbiome and nerve function.
Navigating Diagnosis and Preparing for Medical Consultation
Given the symptom overlap with numerous other gastrointestinal and systemic health conditions, seeking a definitive diagnosis from a credentialed health professional is paramount for anyone suspecting IBS. Conditions such as inflammatory bowel disease, celiac disease, certain infections, food allergies, and even cancer can present with similar symptoms, necessitating careful differentiation to ensure appropriate treatment.
It is particularly crucial to consult a medical professional if any of the following "red flag" symptoms are present: unexplained weight loss, blood in stool, persistent fever, difficulty swallowing, or new onset of symptoms in individuals over the age of 50. These symptoms may indicate more serious underlying conditions requiring immediate medical attention.
During the diagnostic process, healthcare professionals typically utilize criteria like the Rome IV criteria, which define IBS based on recurrent abdominal pain, on average, at least one day a week in the last three months, associated with two or more of the following: related to defecation, associated with a change in frequency of stool, or associated with a change in form (appearance) of stool.
Beyond ruling out other conditions, the healthcare provider will ask detailed questions about the patient’s symptoms to determine the specific IBS "type":
- IBS with Constipation (IBS-C): Predominantly hard or lumpy stools.
- IBS with Diarrhea (IBS-D): Predominantly loose or watery stools.
- IBS with Mixed Bowel Habits (IBS-M): Both hard/lumpy and loose/watery stools.
- IBS Unclassified (IBS-U): Criteria are met, but bowel habits don’t fit into the above categories.
Identifying the specific IBS type guides treatment recommendations. For IBS-D, a healthcare provider might suggest antidiarrheal medications or a short course of antibiotics. For IBS-C, fiber supplements, non-habit-forming laxatives, or medications that reduce pain perception and regulate bowel movements may be recommended.
To maximize the effectiveness of a medical appointment, patients are encouraged to prepare thoroughly. This includes reflecting on questions a healthcare professional is likely to ask, such as:
- When did symptoms begin?
- How often do they occur?
- What triggers seem to worsen them?
- What, if anything, provides relief?
- Are there any associated symptoms like fatigue, anxiety, or depression?
- What medications, supplements, or dietary changes have been tried?
A particularly useful tool for pre-appointment preparation is a "poo diary" kept for a couple of weeks. Tracking bowel movement frequency, symptom severity, and stool quality using the Bristol Stool Chart provides invaluable objective data for the healthcare professional to assess the condition and determine the IBS type. The Bristol Stool Chart categorizes stool consistency from Type 1 (separate hard lumps, difficult to pass) to Type 7 (entirely liquid), offering a visual guide to digestive health.
Holistic Management Strategies for IBS Relief

While the U.S. Food and Drug Administration (FDA) has approved several new prescription medications and medical devices (e.g., cranial nerve stimulators) for IBS in recent years, a vast body of research also highlights the profound impact of lifestyle modifications. These evidence-based strategies not only alleviate IBS symptoms but often contribute to overall health and well-being.
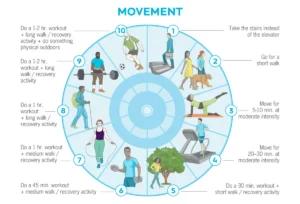
1. Incorporate Regular Exercise:
Individuals with IBS who engage in regular physical activity consistently report fewer symptoms and flare-ups. A study demonstrated that moderate walking for an hour three times a week significantly reduced bloating and abdominal pain within 12 weeks. The exact mechanisms are still being explored, but theories suggest exercise reduces stress and improves mental health, which in turn positively influences the gut-brain axis. Additionally, physical activity may promote the growth of beneficial gut bacteria, enhancing digestion efficiency and reducing inflammation.
2. Prioritize Stress Management:
Stress, anxiety, and depression are potent activators of stress hormones like norepinephrine and cortisol. These hormones can intensify pain signals from the gut, disrupt gut motility, and alter the gut microbiome, exacerbating IBS symptoms. Given that stress is not an "on/off" switch, effective management focuses on cultivating resilience and controlling one’s response to stressors rather than eliminating them. Techniques such as self-compassion, yoga, mindful breathing exercises, and gentle walking can regulate the nervous system, foster calmness, and enhance a sense of control over one’s life, thereby mitigating the physiological impact of stress on the gut.
3. Cultivate Mindful Eating Habits:
Slowing down the eating pace is a foundational strategy for reducing gastrointestinal distress. Mindful, unhurried eating encourages more thorough chewing, which mechanically breaks down food and allows digestive enzymes in saliva to begin the digestion process more effectively. This reduces the workload on the stomach and intestines. Furthermore, eating in a relaxed environment lowers stress hormone levels, making it less likely that they will intensify GI pain signals. For busy individuals, such as young parents, consciously creating a peaceful eating experience can be challenging but highly beneficial.
4. Address Sleep Disturbances:
Poor sleep quality is a common complaint among IBS patients, who often experience more shallow, interrupted, and less restorative sleep. Despite sleeping more hours overall, many report feeling less rested, creating a vicious cycle. Insufficient restorative sleep elevates stress hormone levels, which can exacerbate gut pain. Fatigue also increases hunger and cravings for high-fat, high-sugar foods, which are often IBS triggers, leading to hasty consumption and further digestive upset. While simply "willing" oneself to sleep better is ineffective, implementing the other strategies—exercise, stress management, and mindful eating—can significantly improve sleep quality. Practical tips include consuming a smaller dinner earlier in the evening and establishing a relaxing pre-bedtime routine.
5. Systematically Investigate Dietary Triggers:
While no universal "IBS diet" exists, certain food categories are frequently problematic for a significant portion of patients. These include:
- Fermentable Oligosaccharides, Disaccharides, Monosaccharides, and Polyols (FODMAPs): These short-chain carbohydrates are poorly absorbed in the small intestine. In individuals with IBS, their fermentation by gut bacteria produces excessive gas and draws water into the intestines, leading to intense pain, bloating, and altered bowel habits. High-FODMAP foods include wheat, rye, barley, onions, garlic, certain legumes, dairy products, honey, cashews, and various fruits and vegetables.
- Caffeinated Beverages and Foods: Especially coffee, which can stimulate stomach acid production, increase colon muscle contractions, and irritate the intestinal lining.
- Alcohol and Spicy Foods: Known irritants to the gut lining.
- High Fructose Corn Syrup and Sugar Alcohols (e.g., sorbitol, mannitol): Linked to gas, bloating, and diarrhea in susceptible individuals.
- Fatty, Greasy Foods: Can slow digestion and attract water, contributing to loose stools, bloating, and gas.
It is crucial to recognize that individual sensitivities vary widely. One person might react to apples but tolerate berries, while another might struggle with dairy but enjoy gluten-free options. Therefore, a personalized approach to identifying triggers is essential. This often involves an elimination diet, a structured process to identify problematic foods and the quantities that can be safely tolerated.
The Crucial Role of Health Coaching and Scope of Practice
Health coaches play a vital supportive role in helping individuals manage IBS, particularly in implementing lifestyle and dietary changes. Sarah Maughan, a PN Super Coach certified through Monash University (a global leader in IBS and food sensitivities), emphasizes that coaching clients with IBS falls squarely within a coach’s wheelhouse, provided certain professional boundaries are maintained.
Coaches are empowered to:
- Encourage medical consultation: Always advise clients with digestive issues to seek a definitive diagnosis from a healthcare professional.
- Share information and facilitate experimentation: Provide evidence-based information on lifestyle changes and elimination diets, guiding clients to conduct personal experiments to understand the connection between their habits, diet, and bodily responses.
- Collaborate with medical teams: Offer to work in conjunction with a client’s physician or dietitian, helping the client adopt and maintain consistency with medically recommended lifestyle changes.
- Provide practical tools: Offer recipes, meal ideas, and other resources that support the client in putting their newfound knowledge into practice.
- Promote a multidisciplinary approach: Encourage clients to explore a range of strategies, from medical therapies to lifestyle interventions, to find the most effective combination for their unique needs.
- Empower client choice: Ensure clients understand that they have autonomy over their choices and that information empowers them to make informed decisions about their health.
Conversely, coaches must avoid:

- Diagnosing IBS or any other medical condition.
- Prescribing specific diets as a "cure."
- Contradicting or undermining medical professionals’ advice.
- Creating rigid, prescriptive meal plans for IBS treatment.
- Claiming to have all the answers or implying that medical advice is unnecessary.
- Using fear or manipulation to enforce compliance.
Elimination Diets: A Scientific Approach to Dietary Triggers
Elimination diets are essentially structured "science experiments" designed to identify specific food triggers. They involve temporarily removing certain foods (typically for three weeks) and then systematically reintroducing them one at a time while monitoring symptoms for reactions.
Several types of elimination diets exist, varying in their restrictiveness:
1. Elimination Diet "Lite":
Ideal for individuals who already have a strong suspicion about specific food triggers. This approach involves eliminating up to four suspected foods for a few weeks, then reintroducing them individually to confirm their impact. For example, if dairy is a suspected trigger, it would be eliminated and then reintroduced.
2. Elimination Diet "Medium" (e.g., Precision Nutrition Elimination Diet):
For those less certain of their triggers or seeking a more comprehensive approach without extreme restriction. This plan removes many common problematic foods while ensuring a balanced intake of various vegetables, fruits, starches, legumes, nuts, seeds, and lean proteins. Resources like the "Ultimate Guide to Elimination Diets" provide detailed guidance, including charts, recipes, and meal ideas.
3. The FODMAP Diet:
Developed and extensively researched by Monash University in Australia, the low-FODMAP diet is a highly specialized form of medical nutrition therapy for IBS. Unlike other elimination diets, the list of problematic high-FODMAP foods is complex and non-intuitive, and the reintroduction phase requires careful structuring. Consequently, if a FODMAP issue is suspected, it is strongly recommended to seek guidance from a FODMAP-certified practitioner. Monash University’s FODMAP Diet app is also an invaluable tool for navigating this intricate dietary approach. High-FODMAP foods are categorized by type (oligosaccharides, disaccharides, monosaccharides, polyols), encompassing a wide range of vegetables, fruits, dairy, proteins, starches, sweeteners, nuts, and seeds.
Empowerment Through Knowledge and Ongoing Support
The journey with IBS is often challenging, marked by physical discomfort, psychological strain, and social limitations. The patient reports of willingness to trade years of life expectancy highlight the desperate need for effective solutions and comprehensive support. While knowledge about IBS and its management strategies is crucial, it is the application of this knowledge that truly empowers individuals.
Health coaches, like Sarah Maughan, emphasize that their role extends beyond simply providing information. Many clients may already have an inkling of their food sensitivities but are hesitant to confirm them due to fear of further dietary restrictions. Coaches help clients confront these fears, assuring them that even if a beloved food is identified as a trigger, they retain the choice to consume it or avoid it based on their priorities and the context. This approach fosters a sense of agency and control, transforming knowledge into actionable choices.
The ongoing research into IBS, coupled with a growing understanding of the gut-brain axis and the microbiome, promises future advancements in diagnosis and treatment. In the interim, a holistic approach combining medical care with evidence-based lifestyle interventions, supported by compassionate and knowledgeable health coaching, offers the most promising path toward managing IBS symptoms, reducing gastrointestinal-specific anxiety, and significantly improving the quality of life for millions worldwide. The ultimate goal is to empower individuals with IBS to live the full, vibrant lives they desire, free from the constant shadow of their condition.