For many women navigating the complexities of middle age, a pervasive sense of mental fogginess, emotional instability, and inexplicable fatigue often descends, frequently mistaken for depression or merely the inevitable march of time. This profound shift in cognitive and emotional landscape, as vividly illustrated by personal accounts, signals a critical need for a deeper understanding of menopause, not merely as a reproductive transition but as a significant neurobiological event impacting millions globally. The journey to diagnosis, often protracted and frustrating, highlights systemic gaps in medical education and the persistent underestimation of menopause’s broad physiological and psychological effects.
The Enigma of Brain Fog and Emotional Turbulence
The experience of diminished mental clarity, often described as "brain fog," is a hallmark symptom reported by a substantial portion of women entering perimenopause and menopause. A personal narrative recounts the frustration of a once-sharp individual struggling with basic recall, such as remembering the name of a familiar restaurant. What began as an occasional lapse, typical for middle age, escalated into a debilitating condition by her late 40s and early 50s. This extended beyond simple forgetfulness to a profound inability to concentrate during work hours, a feeling akin to being "barely alive," where even fundamental tasks seemed insurmountable. The author vividly described her thoughts feeling "under a pile of garbage," a common metaphor for the cognitive disarray experienced during this period.
This pervasive mental sludginess was often accompanied by severe emotional disturbances. The individual reported waking with an unshakable haze, rendering work impossible and even leisure activities like reading unattainable. Beyond cognitive struggles, she experienced unprovoked sobbing, heightened sensory sensitivity where normal sounds like traffic became painful, and an uncharacteristic anxiety about everyday situations such as driving. These symptoms, initially dismissed or misdiagnosed, underscore the multifaceted nature of the menopausal transition.
A Diagnostic Odyssey: Misdirection and Missed Clues
The path to understanding these symptoms is frequently fraught with misdirection. In the recounted case, three different healthcare professionals initially recommended antidepressants, a common response to symptoms overlapping with clinical depression. Despite trying several antidepressants and a sleeping pill, the individual’s condition worsened, leaving her feeling "like a zombie" and "even more drugged." Standard medical tests for thyroid function and anemia yielded no answers. A multitude of supplements, from mushroom coffee to various "think" branded products, offered no relief, reflecting a widespread desperation among women seeking solutions.
The breakthrough came nearly two years into this diagnostic odyssey, during a routine gynecological exam. A casual mention of vaginal dryness, a classic menopausal symptom, prompted a series of questions from her gynecologist that finally connected the dots: queries about sleep quality, mood, energy levels, hot flashes, and brain fog. This pivotal conversation illuminated the true underlying cause of her distress: menopause. The subsequent prescription of estradiol and progesterone, components of menopausal hormone therapy (MHT), brought rapid and dramatic relief, akin to "someone had flipped a switch." Within days, cognitive function, sleep patterns, and emotional stability were restored, highlighting the profound hormonal influence on brain health.
Menopause: A Life Stage, Not a Disease, with Significant Health Implications
It is crucial to emphasize that menopause is a natural biological stage in a woman’s life, not a medical condition or disease. Defined as 12 consecutive months without a menstrual period, it marks the end of reproductive years. The preceding phase, perimenopause, and the subsequent postmenopausal stage, are characterized by significant fluctuations and eventual decline in ovarian hormones, particularly estrogen and progesterone. These hormonal shifts are responsible for a wide array of symptoms, far beyond the commonly discussed weight gain and reduced libido.
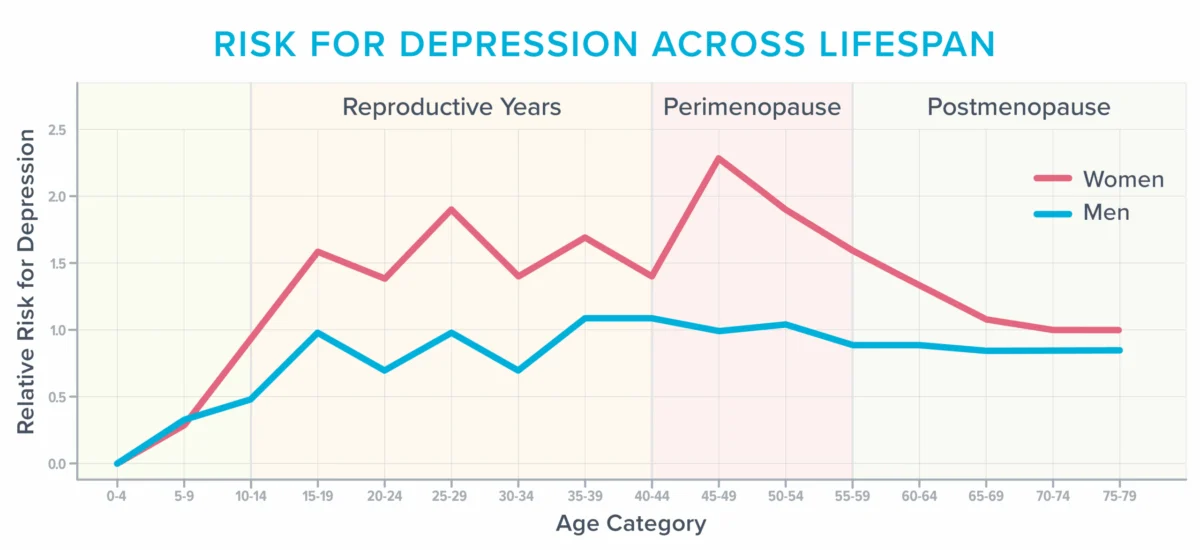
According to the American College of Obstetricians and Gynecologists (ACOG), approximately 40% of women report increased irritability, mood swings, anxiety, fatigue, and trouble concentrating during and after menopause. This period also represents one of the most vulnerable times in a woman’s life for developing depression, especially for those with a prior history of mood disorders. Data illustrate a clear peak in depression risk for women around the perimenopausal years, a trend not observed in men, whose risk remains relatively stable across adulthood. This heightened vulnerability underscores the need for comprehensive screening and appropriate diagnostic approaches during this transitional phase.
The Multifactorial Roots of Cognitive and Emotional Distress
The precise mechanisms driving these cognitive and emotional symptoms are complex, likely involving a combination of fluctuating hormone levels, typical age-related changes in brain structure and function, and significant psychosocial stressors common to women in their 40s and 50s. This demographic often finds itself at the peak of professional careers, juggling demanding responsibilities at work with family caregiving for adolescent children or aging parents, navigating marital changes, or managing significant financial burdens like college tuition or healthcare costs. These life stressors can undoubtedly siphon cognitive and emotional capacity, exacerbating hormonally-driven symptoms.
However, emerging research increasingly points to a specific physiological trigger for cognitive discontent that is directly tied to a hallmark menopausal symptom: the hot flash.
Vasomotor Symptoms: More Than Just an Inconvenience
Hot flashes (daytime) and night sweats (nocturnal) are collectively known as vasomotor symptoms (VMS). These episodes involve the constriction or dilation of blood vessels, influencing blood pressure and sweating. During a VMS event, norepinephrine and cortisol levels surge, blood vessels dilate to shed heat, and heart rate and blood pressure increase. Women may experience skin reddening, sweating, heart palpitations, anxiety, fatigue, or faintness. While the exact cause remains under investigation, one leading theory suggests that falling estrogen levels disrupt the hypothalamus, the brain region responsible for temperature regulation, leading to a "wonky" internal thermostat that misinterprets body temperature.
For years, VMS were largely considered inconvenient or embarrassing but benign. However, a growing body of evidence suggests they are far more significant, potentially impacting blood vessels and brain health adversely. Consequently, many experts now advocate for treating VMS as a medical condition, given their systemic implications.
The Brain-Vessel Connection: Hot Flashes and Cognitive Decline

Research has begun to unravel the detrimental effects of frequent VMS on the brain. One study involving 226 women used monitors to track hot flashes alongside magnetic resonance imaging (MRI) of their brains, sleep diaries, and smartwatch data on nocturnal awakenings. The findings were striking: women who experienced the most hot flashes exhibited a higher prevalence of whole-brain white matter intensities—patchy areas in the brain once considered typical signs of aging. Neuroscientists now recognize these lesions as predictive markers of future cognitive decline, significantly increasing the risk of dementia and stroke.
The underlying mechanism is thought to involve changes in the blood vessels supplying the brain. A three-year study of 492 women corroborated this, showing that frequent hot flashes were associated with unhealthy changes in blood vessel function, specifically an impaired ability to dilate in response to increased blood flow. Other research links frequent hot flashes to increased arterial stiffness, carotid plaque, and elevated markers of inflammation and oxidative stress, all factors contributing to cardiovascular and cerebrovascular disease.
The Sleep-Cognition Axis: Undermining Brain Function
Beyond direct vascular effects, frequent VMS severely disrupt sleep, further compromising brain health. Many women, like the author, may not consciously attribute their sleep disturbances to night sweats, often assuming they have insomnia or sleep apnea. This is because the intense heat of a night sweat may dissipate by the time a surge of cortisol and norepinephrine jolts them awake, leading to repeated, seemingly unprovoked awakenings.
These frequent disruptions prevent the brain from achieving deep, restorative sleep necessary for crucial functions: memory consolidation, detoxification, and the storage of daily information. Chronic sleep loss has been linked to reduced connectivity in the hippocampus, a brain region vital for learning and memory. Furthermore, inadequate sleep can increase the reactivity of the amygdala, the brain’s emotional center, leading to heightened stress, anxiety, irritability, and even rage. These adverse brain changes can manifest within days or weeks of sleep deprivation, compounding over years of chronic sleep disturbance during menopause.
Barriers to Care: Why Diagnosis Remains Elusive
Despite the clear and debilitating impact of menopause, many women struggle to receive appropriate care. Several factors contribute to this systemic challenge:
- Symptom Overlap and Misdiagnosis: The Patient Health Questionnaire (PHQ-9), a common tool for diagnosing depression, includes symptoms like trouble sleeping, feeling tired or having little energy, changes in appetite, and difficulty concentrating—all of which frequently overlap with menopause-related sleep deprivation. Checking off these items can lead to a depression diagnosis, masking the underlying hormonal imbalance.
- Lack of Menopause-Specific Medical Training: A significant barrier is the inadequate education of healthcare professionals regarding menopause. Surveys indicate that 80% of medical residents feel "barely comfortable" discussing menopause, and few residency programs, including OB/GYN, offer comprehensive training in this area. This deficiency means many doctors do not routinely inquire about hot flashes or sleep disturbances when patients present with fatigue, lack of motivation, and cognitive difficulties.
- "Defensive Medicine" and Hormone Therapy Hesitancy: Even when VMS are identified, many healthcare professionals hesitate to prescribe menopausal hormone therapy (MHT), citing concerns about safety and risk. This reluctance, dubbed "defensive medicine" by experts like Dr. Jerrold H. Weinberg, a Michigan-based menopause-trained gynecologist, stems from fears of malpractice lawsuits.
Re-evaluating Hormone Therapy: Current Scientific Consensus
The apprehension surrounding MHT largely originates from research conducted decades ago, which linked certain types of hormones to a slightly increased risk of breast cancer or stroke. However, more recent and nuanced research has refined this understanding. Current evidence suggests that the perceived increased risk depends on several factors, including the woman’s age, the specific dose and type of hormonal preparation used, and the duration of therapy.
The consensus among many experts now is that for women under 60 and those who are fewer than 10 years postmenopausal, the benefits of MHT often outweigh the risks, particularly for moderate to severe menopausal symptoms. Furthermore, MHT offers additional health benefits, such as a reduced risk of Alzheimer’s disease and osteoporosis, according to Dr. Weinberg. While antidepressants can alleviate some menopausal symptoms, they come with their own side effects and do not address the underlying hormonal deficiency or offer the systemic benefits of MHT, making them a "safer bet" for doctors practicing defensively, rather than necessarily the most effective treatment.
Empowering Advocacy: Navigating the Healthcare System
For women struggling with menopausal symptoms, proactive advocacy is paramount. Dr. Weinberg and Helen Kollias, PhD, a physiology and molecular biology expert and science advisor at Precision Nutrition, offer critical advice:
- Seek Menopause-Trained Professionals: Prioritize healthcare providers who explicitly list menopause as an area of focus or who are certified by organizations like The Menopause Society. Databases exist to locate such specialists.
- Document Symptoms Meticulously: Keep a detailed log of symptoms, including their frequency, severity, and impact on daily life. This provides concrete data for appointments, especially when brain fog might impede clear communication. Track hot flashes, night sweats, sleep patterns (duration, awakenings), mood fluctuations, and cognitive issues.
- Be Specific in Communication: Instead of vague statements like "I don’t sleep well," provide precise details: "During the past seven days, I’ve only gotten four uninterrupted hours once. I wake, on average, five times a night. My longest stretch of sleep is typically three hours." Utilize data from smartwatches or health apps if available.
- Engage in Shared Decision-Making: Actively participate in discussions about treatment options, including their benefits and risks. Ask direct questions: "What are the specific benefits and risks of this treatment for me?" "What are the alternatives, and what are their pros and cons?" "How will we monitor the effectiveness and safety of this treatment?" This approach can help shift clinicians away from defensive medicine towards patient-centered care.
Holistic Strategies for Menopausal Well-being
Beyond medical interventions, lifestyle adjustments play a crucial role in managing menopausal symptoms and enhancing overall well-being. While there is no "special diet" for VMS beyond avoiding known triggers like caffeine, alcohol, and spicy foods (and soy products have shown limited efficacy for VMS), fundamental health strategies remain paramount.
- Prioritize Foundational Health: Re-evaluate and reinforce core healthy behaviors:
- Nutrition: Are you consistently eating nutrient-dense whole foods?
- Physical Activity: Are you engaging in regular, appropriate exercise?
- Stress Management: Do you have effective strategies to cope with daily stressors?
- Sleep: Are you prioritizing adequate, restorative sleep?
- Social Connection: Are you maintaining meaningful social relationships?
- Purpose: Do you have a sense of meaning and purpose in your life?
- Consider Creatine Supplementation: Creatine, known for its benefits in muscle and bone health, may also improve mood, bolster brain function, reduce mental fatigue, and counter some negative effects of sleep deprivation. A daily dose of 5-7 grams of creatine monohydrate is often recommended.
- Optimize Light Exposure: Regular exposure to natural light, especially in the morning and late afternoon, helps regulate the body’s internal clock (circadian rhythm), promoting alertness during the day and better sleep at night. Studies show morning sunlight exposure correlates with quicker sleep onset, longer sleep duration, and fewer awakenings.
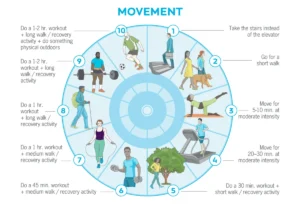
- Moderate Exercise Intensity: While exercise is vital, overly intense or long sessions can exacerbate fatigue and increase injury risk in middle age. Short bursts of movement (e.g., a 5-10 minute walk, a quick set of squats) can boost alertness during the day. Gentle exercises like yoga or stretching can aid relaxation before bed. It’s crucial to listen to your body and adjust workout intensity based on sleep quality and recovery needs, balancing vigorous sessions with moderate activity and adequate rest.
- Explore Cognitive Behavioral Therapy for Insomnia (CBT-I): This evidence-based therapy equips individuals with skills and mental reframes to improve sleep quality. Techniques include maintaining a consistent wake-up time regardless of prior night’s sleep and addressing anxiety around sleep.
- Realistic Stress Management: Acknowledge that energy and bandwidth may be finite. Critically assess responsibilities and identify areas to reduce or delegate. Track time and energy expenditure to pinpoint drains and ask critical questions: "What can I eliminate or simplify?" "What can I ask others to do?" "What am I doing out of obligation versus genuine desire?"
- Utilize Cooling Technology: A cooler sleep environment can significantly reduce night sweats and improve sleep quality. Options include lowering the thermostat, using fans, or investing in electric cooling mattress pads.
- Incorporate Frequent Breaks: When brain fog sets in, productivity plummets. Permitting short breaks (e.g., 20 minutes of quiet rest, gentle stretching, meditation, or a mind-body scan) can help refresh cognitive function. A 5-minute mind-body scan, observing physical sensations and thoughts without judgment, can provide valuable self-awareness and a mental reset.
- Adopt a Circulation-Promoting Diet: Diets rich in vegetables, fruits, whole grains, lean proteins, and healthy fats, such as the Mediterranean and MIND diets, support cardiovascular health and are linked to reduced risks of Alzheimer’s disease and depression. Nitrate-rich foods like beets and dark leafy greens can temporarily improve memory by dilating blood vessels and increasing blood flow to the brain.
The Upside: Re-evaluation and Empowerment
While the challenges of menopause can be profoundly frustrating, this life stage presents a unique opportunity for introspection and re-evaluation. The diminished capacity can force a critical assessment of priorities, prompting questions like, "Do I really need to be doing this?" This existential inquiry can lead to a powerful reassessment of how limited mental and emotional resources are allocated. For the author, it led to a conscious decision to reduce work hours, simplify domestic tasks, and embrace the power of saying "no" to preserve energy for what truly mattered: family, friendships, and personal well-being.
The journey through menopause, though often arduous and misunderstood, can ultimately be a catalyst for profound personal growth and empowerment. With accurate diagnosis, appropriate medical support, and a commitment to holistic lifestyle strategies, women can navigate this transition with greater clarity, vitality, and a renewed sense of purpose, ensuring that their later years are marked by thriving, not merely surviving.