This sentiment resonates deeply with many in an era increasingly focused on extending human healthspan and lifespan. The desire to not only maintain good physical condition but to potentially outlive actuarial age expectancies and remain vibrant, lean, and disease-free into advanced age—90s, 100s, and beyond—is a powerful motivator. However, the prevailing narrative surrounding achieving such a state often presents a daunting challenge: complex longevity advice that demands extraordinary commitments of effort, time, money, and intricate protocols. This raises critical questions about the necessity, efficacy, and ultimate value of such intensive approaches.

The Rise of the Longevity Imperative and the Allure of Optimization
The concept of "health optimization" has exploded into the public consciousness, fueled by a burgeoning longevity industry and influential figures across various platforms. Podcasts, books, and social media feeds are saturated with discussions on biohacking, advanced diagnostic tests, and cutting-edge supplements. Prominent voices like Dr. Peter Attia, Dr. Andrew Huberman, Dr. Rhonda Patrick, and biohacker Bryan Johnson have amplified this movement, presenting highly structured, data-driven regimens designed to push the boundaries of human vitality. The appeal is clear: a longer, healthier life coupled with a comforting sense of control over one’s biological destiny.

Yet, a critical perspective emerges from organizations with extensive real-world experience coaching hundreds of thousands of individuals through their health journeys. For them, the notion of "optimal" health, as often portrayed, is rarely realistic for the average person. More importantly, it’s argued that such extreme optimization isn’t necessary to achieve significant, life-enhancing results. Instead, consistent, modest efforts toward foundational health and well-being are posited to deliver superior outcomes compared to intense, highly optimized, and often unsustainable protocols.
Debunking the Myths of Extreme Longevity

The mainstream longevity conversation is often underpinned by several pervasive myths that can mislead individuals and create unnecessary barriers to genuine health improvement.
Myth 1: The "Basics" Are Insufficient for Longevity.
There’s a common misconception that achieving exceptional health and extending lifespan requires a suite of complex, "cutting-edge" strategies. The reality, supported by decades of public health research, is that foundational health behaviors are remarkably effective. These include regular exercise, a nutrient-rich diet, adequate sleep, effective stress management, and strong social connections. The primary challenge isn’t the lack of sophisticated interventions but the widespread inconsistency in adhering to these relatively simple practices. For instance, few people consistently meet recommended guidelines for daily fruit and vegetable intake, sleep duration, or combined aerobic and resistance exercise. The true gap in public health outcomes often lies not in missing exotic treatments but in failing to consistently implement well-established, health-promoting behaviors. Individuals consistently practicing a well-rounded set of these habits with 80-90% fidelity are likely already near peak optimization in terms of broad health benefits.

Myth 2: More Effort Always Equates to Better Results.
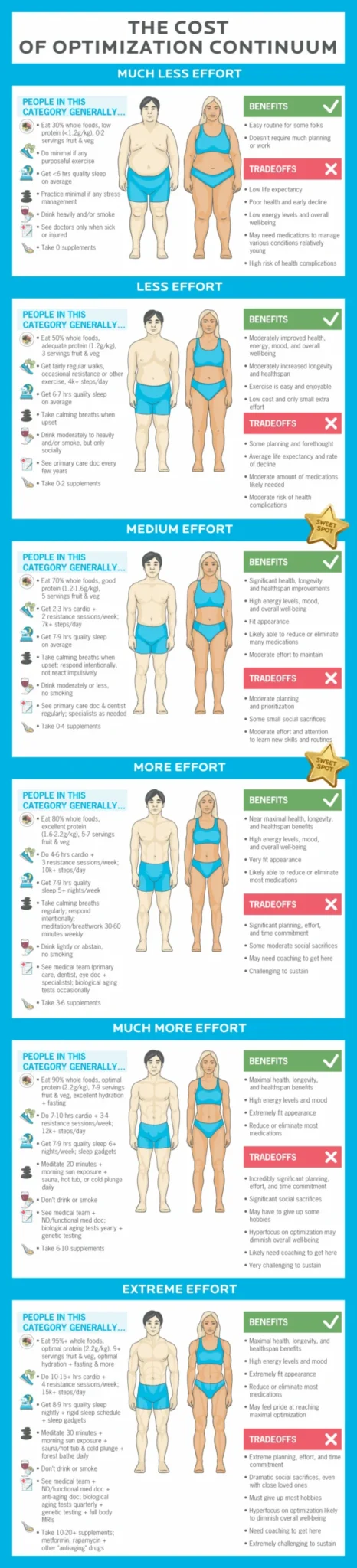
While a certain level of effort is crucial, the relationship between health efforts and longevity benefits follows a law of diminishing returns. Initial investments in basic health habits yield substantial improvements. However, as efforts become increasingly intense and complex, the incremental benefits shrink, while the associated costs (time, money, psychological burden) escalate. Pushing beyond a certain point can lead to burnout, decreased adherence, and a diversion of resources from other life-enriching activities. The goal of a long life shouldn’t overshadow the importance of living a full, enjoyable life, suggesting that an optimal balance exists rather than a linear "more is better" trajectory.
Myth 3: Cutting-Edge Strategies Offer Significant, Proven Benefits.
Many of the advanced, complex strategies promoted within optimization circles lack robust scientific validation in human populations. Much of the supporting research is often limited to animal models, observational studies, theoretical frameworks, or small-scale human trials of short duration. Fringe methods and supplements touted by influencers often remain unproven, and some can even carry potential safety risks. Prioritizing efforts toward foundational health behaviors with established efficacy is a more prudent and evidence-based approach than investing in unverified interventions.

Myth 4: Health is an "All-or-Nothing" Endeavor.
The perceived overwhelming nature of "optimizing" health can lead some to paralysis, believing that if they cannot achieve perfection, any effort is futile. This "all-or-nothing" mindset is counterproductive. Data from large-scale coaching programs demonstrates that even clients who adhere to basic habits less than half the time achieve measurable and significant health improvements. This underscores that incremental progress and moderate consistency are powerful drivers of positive change, making great health accessible even without perfect adherence.
The Foundational Pillars of a Long, Healthy Life

Instead of chasing elusive "optimality," focus on these evidence-backed foundational behaviors, understanding their "sweet spot" of effort versus reward.
1. Exercise: The Cornerstone of Vitality
Physical activity is universally recognized as crucial for health and longevity. It extends lifespan, reduces the risk of chronic diseases (cancer, cardiovascular disease, diabetes), and improves mood, energy, and cognitive function. Studies, including those on Harvard alumni, consistently show that any amount of physical activity reduces mortality risk, independent of other factors. Significant risk reductions are observed with as little as 7.5 to 15 MET-hours of activity per week, with benefits plateauing thereafter. Even daily walking—with every 1,000-step increase linked to a 12% lower risk of death—demonstrates profound impact. For cognitive health, just 3,826 steps daily can reduce dementia risk by 25%.

Combining cardiovascular activity with resistance training is ideal. Resistance training preserves muscle mass (combating sarcopenia), enhances bone density, improves balance (reducing fall risk, a leading cause of death in older adults), supports metabolic health, and aids mental sharpness. A sedentary lifestyle, conversely, doubles the risk of premature death over two decades.
- Optimal Dose: Aim for at least 150 minutes of moderate-intensity or 75 minutes of vigorous-intensity aerobic activity per week, plus two or more resistance training sessions targeting all major muscle groups. Further benefits accrue up to 300 minutes aerobic and three resistance sessions.
- Current Adherence: Only 24% of Americans meet both aerobic and resistance guidelines; fewer than 47% meet aerobic recommendations.
- More is Better? Benefits typically max out around 7-10 hours of cardio and 3-4 resistance sessions per week. Excessive exercise can lead to overtraining syndrome (hormonal disruption, fatigue, injuries) and potentially adverse cardiac effects, illustrating the "Extreme Exercise Hypothesis" where risks are lowest at moderate-to-high levels, not extreme.
2. Nutrition: Fueling a Longer Life
A nourishing diet need not be complex, focusing on three key fundamentals:

-
Prioritize Whole and Minimally-Processed Foods: These foods are naturally rich in fiber, healthy fats, vitamins, minerals, and phytochemicals, while being less calorie-dense and lower in sugar, sodium, and trans fats. Diets rich in these foods are linked to lower rates of depression, heart disease, type 2 diabetes, cancer, and improved longevity. Conversely, ultra-processed foods (UPFs) are associated with 32 harmful health effects, including a 62% increased risk of all-cause mortality with four or more servings daily.
- Optimal Dose: Aim for 70-80% of your diet from whole or minimally-processed foods. Even 50% can yield significant benefits.
- Current Adherence: Americans derive only 28.5% of calories from whole/minimally-processed foods, with 56% from UPFs.
- More is Better? Consuming up to 90% from minimally-processed foods maximizes benefits, but beyond that, gains are negligible, and some processed foods (e.g., protein powder) can be health-enhancing.
-
Consume Five Servings of Fruits and Vegetables Daily: This widely echoed advice is backed by robust evidence. A meta-analysis of 1.8 million people found that five servings daily correlated with a 13% lower risk of death from any cause, with benefits plateauing at this level. Fruits and vegetables reduce risks of hypertension, heart disease, stroke, and possibly cancer and weight gain.

- Optimal Dose: Five fist-sized servings daily (e.g., three vegetables, two fruits), ideally with a variety of colors to maximize phytonutrient intake.
- Current Adherence: Americans average 2.5 servings daily; only 10% meet the five-serving recommendation.
- More is Better? Life-extending benefits plateau at five servings. While more won’t harm and offers other benefits (satiety), it doesn’t yield additional mortality risk reduction.
-
Ensure Adequate Protein Intake: Protein is critical, especially with age, to combat sarcopenia, maintain muscle mass, support bone health, immunity, and satiety. Plant proteins are linked to reduced cardiovascular disease and all-cause mortality. For animal proteins, minimally processed fish, poultry, and low-fat dairy are preferred. Processed red meats should be limited, and even unprocessed red meat to about 18 oz/week.
- Optimal Dose: Minimum of 1.2 g/kg body weight for most adults, particularly older individuals and those on GLP-1 medications. 1.6-2.2 g/kg is optimal for muscle growth, strength, and vigorous exercise recovery.
- Current Adherence: Most adults meet the lower 0.8 g/kg recommendation, but up to 46% of older adults may not. The ideal intake is often higher than typically consumed.
- More is Better? Benefits largely plateau around 1.2 g/kg for sedentary individuals, with marginal gains up to 2.2 g/kg for highly active or specific populations.
3. Sleep: The Restorative Imperative
Quality sleep is as fundamental as exercise and diet for health and longevity. Men getting adequate sleep live nearly five years longer, and women 2.5 years longer. Sleep is vital for heart health, reducing cardiovascular disease and type 2 diabetes risk. Deep sleep clears beta-amyloid plaques, crucial for preventing dementia and cognitive decline.

- Optimal Dose: 7-9 hours per night for most adults, with at least 7 hours on most nights, allowing for refreshed waking and sustained daytime energy.
- Current Adherence: Approximately one-third of US adults fall short of 7-9 hours.
- More is Better? Sleeping consistently over 9 hours is associated with increased risks of cardiovascular disease and type 2 diabetes, though this may reflect underlying health issues rather than direct causation. The 7-9 hour window appears optimal.
4. Stress Management: Cultivating Resilience
Chronic, unmanaged stress negatively impacts nearly every bodily system, increasing heart rate, blood pressure, inflammation, and risk of cardiovascular disease, anxiety, and depression. However, stress isn’t inherently bad; appropriate levels foster motivation and engagement. Effective stress management involves developing healthy coping mechanisms and resilience.
- Strategies: Mindset shifts (self-compassion, growth mindset, reframing stress), self-regulation skills (noticing emotions, controlled actions), and recovery practices (deep breathing, journaling, nature exposure).
- Optimal Dose: Proportional to life’s demands. Even 3-5 minutes of purposeful recovery can be beneficial. The goal is to find a "sweet spot" where one feels energized and engaged, not overwhelmed or bored.
- Current Adherence: Over a quarter of people in the US and Canada report stress levels that impair function, and over a third don’t know where to start with stress management.
- More is Better? Beyond the "sweet spot" of feeling energized and engaged, adding more stress reduction techniques can become another burden, leading to diminishing returns.
5. Social Connection: The Power of Human Bonds
Social connection is a critical health imperative, often overlooked in physical health discussions. Strong social and emotional support is linked to improved well-being and a 50% increased likelihood of survival. The Harvard Study of Adult Development, spanning over 87 years, identified strong relationships as the biggest predictor of life satisfaction and longevity, surpassing wealth, IQ, or genetics. Conversely, social isolation and loneliness increase risks for heart disease, stroke, diabetes, depression, dementia, and premature death, with an impact comparable to smoking 15 cigarettes daily.

- Optimal Dose: Having 3-5 close friends with whom one interacts regularly (1-3 times/week, in-person or by phone) tends to provide the most social benefit. Quality over quantity is key.
- Current Adherence: Approximately 1 in 3 adults report loneliness, and 1 in 4 lack social support. 8% report no close friends.
- More is Better? Excessive social engagement (daily or multiple times daily) might increase mortality risk due to increased fatigue, potential for risky behaviors, and displacement of other essential health habits.
6. Minimizing Harms: Avoiding the Obvious Threats
Actively avoiding known harms is a non-negotiable aspect of long-term health.
- Don’t Smoke: Tobacco use remains a leading preventable cause of death globally, accounting for over 8 million premature deaths annually. It is a major risk factor for coronary heart disease, stroke, emphysema, and various cancers (25% of cancer deaths attributed to smoking).
- Current Prevalence: Despite widespread awareness, 12% of US adults (28 million people) smoke, and globally, 1.3 billion people use tobacco.
- Limit Alcohol Consumption: Research unequivocally links alcohol to negative health outcomes, particularly with regular heavy use. Alcohol plays a causal role in over 200 diseases, including liver diseases, heart diseases, seven types of cancers, depression, and dementia. It was responsible for 2.6 million deaths worldwide in 2019 and is the leading risk factor for death among 15-49 year olds.
- Optimal Dose: US guidelines suggest moderate intake: up to one drink per day for women, up to two for men (a "drink" being 14g ethanol, e.g., 12oz beer, 5oz wine, 1.5oz spirits). The WHO states no amount is "safe," but risk is non-linear, rising exponentially with heavy drinking. The lowest risk is achieved with minimal to no intake.
- Current Adherence: Americans typically consume more than recommended, with heavy episodic drinking common.
- More Abstinence is Better? From a purely physical health perspective, abstinence is ideal as alcohol is a carcinogen. However, social and cultural factors exist. Intentional decisions based on understanding risks (which rise significantly with heavy drinking: 4+ drinks/day for women, 5+ for men, or 8+/week for women, 15+/week for men) are key.
7. Basic Preventive Health Measures: The Unsung Heroes
Often mundane but immensely impactful, these measures protect health over a lifetime. They include routine medical check-ups, vaccinations, dental hygiene, vision and hearing tests, medication adherence, helmet use for cycling, seatbelt use, sunscreen application, and safe driving. Hearing loss, for example, is the number one modifiable risk factor for dementia.

- Optimal Dose: Consistent adherence to public health recommendations and personal safety practices. Regular check-ups and addressing lingering health concerns are crucial.
- Current Adherence: While seatbelt usage is high (~92%), only 32% of Americans floss daily, and about half of cyclists wear helmets. Many neglect hearing protection.
- More is Better? Obsessive risk elimination is impractical. Reasonable, consistent efforts in these areas contribute immeasurably more to overall health than chasing optimization fads.
Bonus: Fostering a Sense of Purpose and Meaning
Beyond physical and behavioral habits, a strong sense of purpose and meaning in life is consistently linked to improved health, well-being, and longevity. This "existential boost" offers a unique benefit distinct from mere happiness, driving individuals to engage in health-promoting behaviors and improving mental health (e.g., 43% reduced depression risk). It fundamentally makes people want to live longer to fulfill their aims, whether through career, relationships, creative pursuits, or community involvement.
The Significant Trade-offs of Extreme Optimization

While foundational habits yield substantial returns, pushing for "optimal" often entails exponential increases in effort for marginal, uncertain gains.
Time and Financial Investment: An "optimizer" lifestyle demands significantly more time and money than a simply "healthy" one. Weekly expenditures can be 3-4 times higher, encompassing extended exercise regimens, specialized dietary preparations, elaborate recovery protocols (e.g., red light therapy, cryotherapy, hyperbaric oxygen), and a host of unproven supplements. Beyond weekly routines, monthly or annual interventions like advanced blood tests, genetic sequencing, bespoke coaching, and experimental therapies can easily add $10,000+ per year. This creates a substantial barrier, making "optimization" a privilege often reserved for the wealthy.

Impact on Well-being and Quality of Life: The pursuit of extreme optimization can paradoxically detract from overall well-being. Excessive focus on physical health can compromise other aspects of "deep health"—relational, emotional, existential, mental, and environmental. The relentless pursuit of perfection can foster orthorexia (an unhealthy obsession with healthy eating) or other mental health conditions. A life dominated by rigid protocols, constant tracking, and anxiety over minor deviations risks sacrificing spontaneity, joy, and meaningful human connection. True health encompasses not just biological longevity but also the richness and satisfaction derived from living a full, balanced, and enjoyable life.
Making Informed Choices for Your Health Journey

Navigating the complex landscape of health and longevity requires clarity and self-awareness.
- Clarify Your Goals: Reflect on what truly constitutes a "good life" for you. How important is maximizing healthspan and lifespan relative to other life priorities, such as relationships, career, or personal passions?
- Consider the Trade-offs: Be realistic about the time, money, and effort you are willing and able to invest. What aspects of your life are you prepared to adjust or sacrifice, and what are non-negotiable?
- Start with the Basics: Objectively assess your adherence to the foundational health behaviors outlined in this article. If there are gaps, prioritize improving consistency in these areas first. These efforts will deliver the most significant and reliable returns.
- Tune Out the Noise: Remember that external "experts" and influencers don’t dictate your personal health journey. Empower yourself to make choices aligned with your values, resources, and what genuinely contributes to your well-being.
Ultimately, a long, healthy, and fulfilling life is largely achieved not through extreme, expensive, and often unproven "optimization" fads, but through consistent, practical commitment to fundamental health behaviors. It’s a journey of sustainable habits, informed choices, and a balanced perspective that values both longevity and the joy of living.