The experience described as having thoughts "under a pile of garbage," a frustrating inability to recall proper nouns, and a pervasive mental haze during daily tasks, is a narrative resonating with a growing number of women entering their late 40s and early 50s. Far from being a mere inconvenience or a typical sign of aging, these cognitive and emotional disturbances, often misdiagnosed as depression or anxiety, are increasingly being recognized as significant symptoms of the menopausal transition, profoundly impacting quality of life, professional productivity, and overall well-being. This article delves into the complex interplay between hormonal shifts, neurological changes, and societal understanding that often leaves women navigating a diagnostic odyssey, only to discover that their struggles are rooted in menopause, not mental illness.
The journey often begins subtly, as detailed in one woman’s account of a once-simple Friday night dinner decision. What should have been an easy choice became an exercise in mental gymnastics, a frustrating attempt to retrieve a restaurant name lost in a "pile of sludge" in her brain. This "sludginess," particularly with proper nouns, is often dismissed as a benign aspect of middle age. However, for many, the cognitive decline extends beyond occasional forgetfulness, manifesting as a debilitating brain fog that infiltrates professional and personal life. Days begin with a mental haze that refuses to lift, rendering complex tasks impossible and even basic activities like reading or engaging in conversation feel like insurmountable challenges. This profound cognitive impairment, coupled with overwhelming fatigue and a lack of drive, often leads individuals to seek medical help, only to be met with a series of misdiagnoses.
The Diagnostic Labyrinth: When Menopause Masquerades as Depression
The initial medical consultations frequently point towards mental health conditions. In the illustrative case, three healthcare professionals recommended antidepressants, and a fourth prescribed sleeping pills, none of which alleviated the symptoms. In fact, some treatments exacerbated the feelings of lethargy and detachment, transforming the patient into what she described as a "zombie." Standard tests for thyroid function and anemia yielded no answers, and a host of over-the-counter supplements and purported brain-boosting products proved equally ineffective. This prolonged "diagnostic odyssey," lasting nearly two years for some, highlights a significant gap in medical training and awareness surrounding menopause.
The breakthrough often comes unexpectedly, triggered by an unrelated symptom. In this instance, a routine gynecological exam and a mention of vaginal dryness prompted a series of questions that finally connected the dots: sleep patterns, mood, energy levels, hot flashes, and critically, brain fog. The realization that the profound cognitive and emotional distress was not depression but, in fact, menopause, marks a pivotal moment. Prescriptions for estradiol and progesterone, components of menopausal hormone therapy (MHT), led to a dramatic and rapid improvement. Within days, the mental clarity returned, work became manageable, conversations were engaging, and, perhaps most crucially, uninterrupted sleep became a reality after years of fragmented rest.
Menopause: A Life Stage with Profound Systemic Impacts
Menopause is not a disease or a medical condition but a natural biological transition, marking the end of a woman’s reproductive years. It is officially diagnosed after 12 consecutive months without a menstrual period, signifying the cessation of ovarian function and a dramatic decline in estrogen and progesterone production. This transition, preceded by a phase known as perimenopause, typically begins in a woman’s 40s and can last for several years, characterized by fluctuating hormone levels that trigger a wide array of symptoms. While common symptoms like weight gain, reduced sex drive, and hot flashes (vasomotor symptoms) receive considerable attention, the cognitive and emotional impacts are often underestimated and under-recognized.
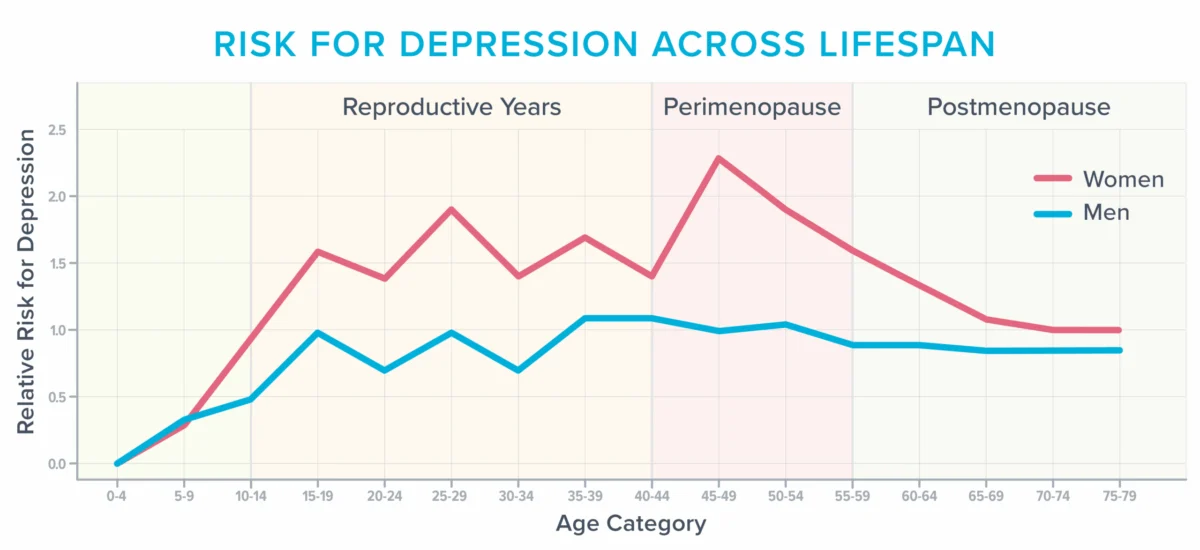
According to the American College of Obstetricians and Gynecologists (ACOG), approximately 40 percent of women experience increased irritability, mood swings, anxiety, fatigue, and difficulty concentrating during and after menopause. The hormonal shifts during perimenopause and menopause, particularly the decline in estrogen, have a direct impact on brain function. Estrogen plays a crucial role in regulating neurotransmitters, promoting neuronal health, and influencing cerebral blood flow. Its decline can therefore affect memory, executive function, and emotional regulation. Furthermore, research indicates that the perimenopausal years represent a period of heightened vulnerability for the development of depression, especially in women with a history of mood disorders. This is clearly illustrated by epidemiological data showing a peak in depression risk for women around the perimenopausal age, contrasting with a relatively stable and lower risk for men across adulthood.
Beyond the direct hormonal effects, this life stage often coincides with significant psychosocial stressors. Women in their 40s and 50s are frequently at the peak of their careers, shouldering immense professional responsibilities. Simultaneously, they may be navigating the complexities of parenting teenagers, caring for aging parents, adjusting to an "empty nest," or dealing with financial pressures. These external demands can further compound the cognitive load and emotional strain, making it challenging to discern the root cause of declining mental function.
The Stealthy Saboteur: Vasomotor Symptoms and Brain Health
One of the most insidious and often overlooked triggers for cognitive and emotional distress during menopause is the hot flash (and its nocturnal counterpart, night sweats). These vasomotor symptoms, characterized by the constriction and dilation of blood vessels, are more than mere inconveniences; they are increasingly viewed as a treatable medical condition with tangible impacts on cardiovascular and brain health.
During a hot flash or night sweat, there is a surge in norepinephrine and cortisol, leading to rapid physiological changes: blood vessel dilation, increased heart rate, and elevated blood pressure. This cascade can cause skin reddening, sweating, palpitations, and feelings of anxiety or faintness. While the exact mechanisms remain under investigation, one leading theory suggests that falling estrogen levels disrupt the hypothalamus, the brain’s thermoregulatory center, leading to a "wonky" internal thermostat that misinterprets body temperature.
Emerging research highlights the profound impact of vasomotor symptoms on the brain. A study involving 226 women found a strong correlation between frequent hot flashes and an abundance of "whole-brain white matter intensities" observed on MRI scans. These patchy areas, once considered a normal part of aging, are now understood as predictive markers for future cognitive decline, increasing the risk of dementia twofold and stroke threefold. This suggests that frequent hot flashes may contribute to microvascular damage in the brain. Supporting this theory, a three-year study of 492 women revealed that those experiencing frequent hot flashes also exhibited unhealthy changes in their blood vessels, including impaired endothelial function and reduced ability to dilate in response to increased blood flow. Other research has linked frequent hot flashes to increased oxidative stress, inflammation, and insulin resistance, all of which can negatively impact brain health.

Furthermore, vasomotor symptoms are a major disruptor of sleep. Night sweats, even when not overtly "sweaty," can trigger surges of cortisol and norepinephrine that repeatedly jolt women awake. These micro-arousals often go unnoticed, leading women to believe they have generic insomnia or sleep apnea, rather than recognizing the underlying hormonal cause. Chronic sleep deprivation, even for a few days, has significant repercussions for the brain. It impairs the brain’s ability to consolidate memories, clear metabolic toxins (via the glymphatic system), and process daily information. It can also lead to reduced connectivity in the hippocampus, a critical region for learning and memory, and increased reactivity in the amygdala, contributing to heightened stress, anxiety, irritability, and rage. The cumulative effect of years of such disturbed sleep can be devastating for cognitive and emotional well-being.
Barriers to Care: Systemic Challenges in Menopause Management
Despite the clear and debilitating nature of menopausal symptoms, many women struggle to receive appropriate care. One significant hurdle lies in the diagnostic tools used for mental health. The Patient Health Questionnaire (PHQ-9) depression scale, widely used by healthcare professionals, includes several symptoms that overlap significantly with menopause-related sleep deprivation, such as trouble sleeping, feeling tired or having little energy, changes in appetite or overeating, and difficulty concentrating. Checking off just four of these nine symptoms can lead to a depression diagnosis, potentially diverting attention from the underlying hormonal imbalance.
Another critical systemic issue is the widespread lack of menopause-specific training within the medical community. Surveys reveal that 80 percent of medical residents feel "barely comfortable" discussing menopause, and few residency programs, including those for obstetricians and gynecologists, offer comprehensive training in this area. This educational deficit means that many healthcare professionals do not routinely inquire about hot flashes or sleep disturbances when women present with symptoms like fatigue, brain fog, and lack of motivation.
Even when vasomotor symptoms are clearly identified as contributing to cognitive and emotional issues, a reluctance to prescribe menopausal hormone therapy (MHT) persists among many healthcare providers. This hesitancy often stems from historical concerns, primarily related to the Women’s Health Initiative (WHI) study conducted decades ago, which linked certain types of hormones to a slightly increased risk of breast cancer and stroke. However, more recent and nuanced research has clarified that the risks associated with MHT are highly dependent on factors such as age, dose, type of hormonal preparation, and duration of use.
Leading medical organizations, including the Menopause Society (formerly NAMS) and ACOG, now advocate that for women under 60 or within 10 years of menopause onset, with moderate to severe symptoms, the benefits of MHT often outweigh the risks. These benefits include not only symptom relief but also potential long-term health advantages such as a reduced risk of Alzheimer’s disease and osteoporosis. Dr. Jerrold H. Weinberg, a Michigan-based menopause-trained gynecologist, attributes much of the medical community’s reluctance to "defensive medicine," where the fear of malpractice lawsuits influences treatment decisions. While antidepressants can offer some relief for mood and hot flashes, they come with their own side effect profiles and do not address the root hormonal cause of menopause-related cognitive symptoms.
Empowering Advocacy: Navigating the Healthcare System
For women navigating the complexities of menopause, proactive self-advocacy is paramount. Experts like Dr. Weinberg and Helen Kollias, PhD, a physiology and molecular biology expert, offer practical strategies:
- Seek Menopause-Trained Professionals: Prioritize healthcare providers who explicitly list menopause as an area of focus or hold certifications from organizations like the Menopause Society (e.g., through their online database).
- Document Symptoms Meticulously: Keep a detailed log of symptoms, including their frequency, severity, and impact on daily life. This provides concrete data for discussions with healthcare providers, especially when brain fog might impair recall during appointments. Track sleep patterns (duration, awakenings), hot flash episodes, mood fluctuations, energy levels, and cognitive challenges.
- Be Specific in Communication: Vague statements like "I don’t sleep well" are less impactful than precise descriptions such as, "Over the past week, I’ve had only one night of uninterrupted sleep for more than four hours. I wake up, on average, five times a night, with my longest stretch of sleep being three hours." Utilize data from smartwatches or sleep trackers to provide objective evidence.
- Engage in Shared Decision-Making: Actively participate in discussions about treatment options, including the benefits and risks of MHT. Ask questions such as: "What are the specific risks and benefits of this treatment for me, given my health history and age?" and "Are there alternatives, and what are their pros and cons?" This collaborative approach can help shift a clinician away from a purely defensive mindset.
Holistic Strategies for Mental and Emotional Well-being During Menopause
While medical intervention can be transformative, a comprehensive approach to managing menopause also integrates lifestyle strategies. These fundamental health habits, crucial at any life stage, become even more critical during this transition:
- Prioritize Fundamental Health Strategies: Re-evaluate and reinforce foundational pillars:
- Nutrition: Focus on a balanced diet rich in whole foods, lean proteins, healthy fats, and fiber.
- Physical Activity: Regular movement tailored to current energy levels.
- Stress Management: Implement techniques to mitigate chronic stress.
- Quality Sleep: Optimize sleep hygiene and environment.
- Social Connection: Maintain strong relationships and community engagement.
- Sense of Purpose: Engage in activities that bring meaning and fulfillment.
- Experiment with Creatine: Beyond its known benefits for muscle and bone health, 5-7 grams of creatine monohydrate daily may improve mood, cognitive function, reduce mental fatigue, and even counteract some negative effects of sleep deprivation by supporting brain energy metabolism.
- Optimize Light Exposure: Regular exposure to natural light, particularly in the morning and late afternoon, helps regulate the circadian rhythm, promoting alertness during the day and better sleep at night. Sunlight also has mood-enhancing and concentration-boosting effects.
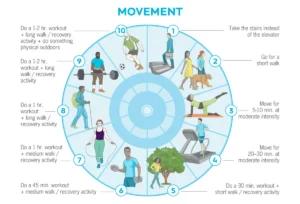
- Adjust Exercise Intensity: During menopause, recovery times lengthen, and injury risk increases. While movement is vital, intense, long exercise sessions may exacerbate fatigue and irritability. Incorporate short bursts of movement (5-10 minute walks or bodyweight exercises) for alertness and gentle exercises like yoga for relaxation. Balance intense workouts with moderate sessions and prioritize proportionate recovery.
- Investigate Cognitive Behavioral Therapy for Insomnia (CBT-I): This evidence-based therapy teaches skills and cognitive reframing techniques to improve sleep, such as consistent wake times and addressing sleep-related anxiety.
- Realistically Assess and Manage Stress: Conduct an inventory of responsibilities and commitments. Identify areas where demands can be reduced, delegated, or eliminated. Tools like a "Wheel of Stress Assessment" can help pinpoint specific stressors, enabling targeted interventions and the courage to set boundaries.
- Utilize Cooling Technology: A cooler sleep environment can significantly reduce night sweats and improve sleep quality. This can involve lowering the thermostat, using fans, or investing in cooling mattress pads.
- Incorporate Frequent Breaks and Mindfulness: When brain fog sets in, productivity plummets. Short breaks (20 minutes of complete disengagement, light stretching, or a mind-body scan) can help reset cognitive function and reduce mental fatigue.
- Adopt a Circulation-Promoting Diet: Diets like the Mediterranean and MIND diets, rich in vegetables, fruits, whole grains, lean proteins, and healthy fats, support cardiovascular health, which directly impacts brain blood flow and function. Nitrate-rich foods such as beets and dark leafy greens can temporarily improve memory by promoting blood vessel dilation and increasing cerebral blood flow.
The Transformative Potential of Menopause
While the challenges of menopause can be profoundly frustrating, this life stage also presents a unique opportunity for introspection and re-evaluation. The forced slowdown and cognitive limitations can compel women to critically assess their priorities and allocate their finite mental and physical resources more judiciously. For many, this leads to a powerful realization: the need to relinquish the pressure to "do it all."
By embracing the changes and making conscious choices, women can redefine their professional and personal boundaries. This might involve adjusting work hours, simplifying domestic tasks, or consciously saying "no" to non-essential commitments without guilt. This newfound clarity allows for a deliberate shift towards prioritizing relationships, personal well-being, and activities that bring genuine joy and fulfillment—whether it’s spending more time with family, pursuing hobbies, or simply enjoying moments of quiet reflection. With appropriate medical support and thoughtful lifestyle adjustments, women can navigate menopause not just to mitigate its challenges, but to emerge with renewed energy, sharper focus, and a profound sense of purpose and agency, reclaiming their cognitive vitality and charting a more intentional path forward.