For many women, the transition into middle age ushers in a baffling array of cognitive and emotional challenges often mistaken for depression or general aging. This often-overlooked reality is vividly illustrated by personal accounts of profound mental "sludginess," where simple tasks like recalling a restaurant name become Herculean efforts. What begins as frustrating forgetfulness, particularly with proper nouns, can escalate into a pervasive brain fog, impacting daily function, professional productivity, and overall quality of life. This cognitive decline, frequently dismissed or misdiagnosed, is increasingly recognized as a significant symptom of menopause, demanding a re-evaluation of current medical approaches and a deeper understanding of its underlying physiological mechanisms.
The experience of feeling mentally incapacitated, where thoughts are obscured "under a pile of garbage," is a common, yet frequently unheard, lament among women approaching and experiencing menopause. A seemingly innocuous Friday night conversation, struggling to recall the name of a familiar restaurant ("Texas Roadhouse!"), can symbolize a much deeper issue. This wasn’t merely age-related forgetfulness; for many, it signals a profound shift in cognitive function that feels "far from typical." Beyond struggling to retrieve names of people, places, or media, the brain fog can manifest as a crippling inability to focus during the workday, a persistent mental haze that resists all attempts to shake it off. This state often leaves individuals feeling "barely alive," unable to engage in work, leisure, or even basic self-care.
The Pervasive Problem of Misdiagnosis
The journey to understanding these symptoms is often fraught with misdirection within the healthcare system. Many women, presenting with fatigue, lack of motivation, and cognitive difficulties, are initially directed towards mental health solutions. Prescriptions for antidepressants, often tried sequentially and at varying doses, can exacerbate symptoms, leaving patients feeling like "zombies" or "even more drugged." Diagnostic tests for common physical ailments like thyroid issues or anemia frequently yield normal results, further deepening the mystery and frustration. The pursuit of relief can lead to an exploration of various supplements, nootropics, and lifestyle changes, all while the root cause remains unaddressed.
The turning point for many arrives unexpectedly, often during routine gynecological examinations, where seemingly unrelated symptoms like vaginal dryness prompt a more comprehensive inquiry into sleep patterns, mood, energy levels, hot flashes, and critically, brain fog. It is in these moments that the realization dawns: the debilitating symptoms are not depression, but rather manifestations of menopause. This underscores a critical gap in medical training and patient care, where the systemic impact of hormonal shifts during menopause is frequently overlooked in favor of more generalized or psychiatric diagnoses.
Menopause: A Life Stage, Not a Disease, with Profound Impacts
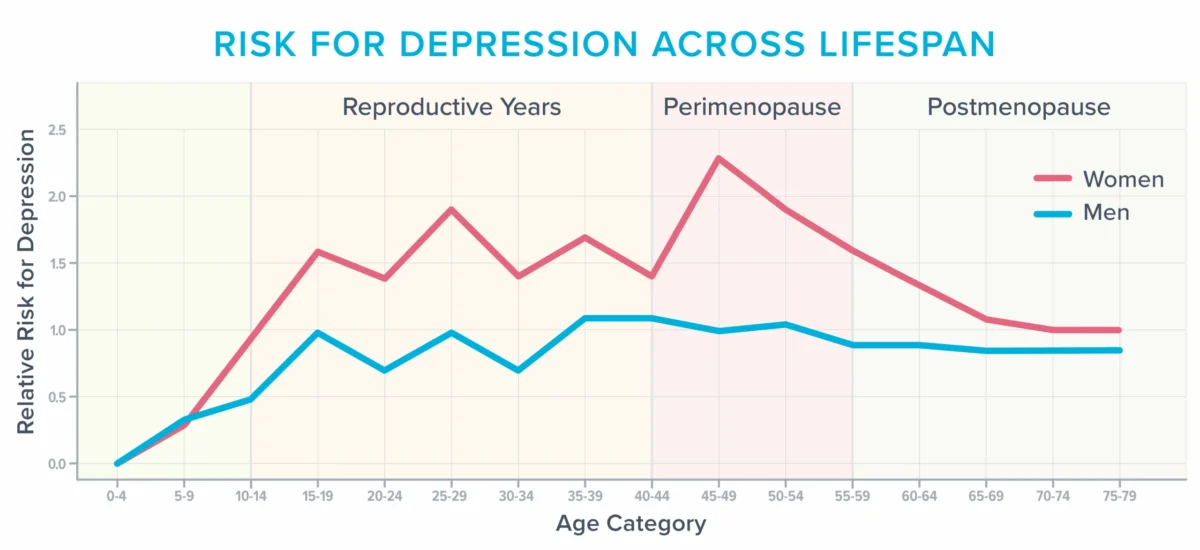
Menopause itself is not a medical condition or a disease, but a natural biological stage in a woman’s life, marking the cessation of menstrual periods and the end of reproductive years. It is clinically defined as 12 consecutive months without a period. The preceding period, known as perimenopause, can last for several years, characterized by fluctuating and eventually declining hormone levels, primarily estrogen and progesterone. These hormonal shifts trigger a wide array of symptoms, some widely discussed like weight gain and reduced sex drive, and others less so, particularly those affecting cognitive and emotional health.
Indeed, during and after menopause, approximately 40% of women report increased irritability, mood swings, anxiety, fatigue, and trouble concentrating, according to the American College of Obstetricians and Gynecologists. The perimenopausal years also represent a particularly vulnerable period for the development of depression, especially for women with a history of mood disorders. Beyond the cognitive struggles, emotional volatility can manifest as unexplained crying spells, heightened sensory sensitivity where everyday sounds become painful, and pervasive anxiety about previously innocuous situations. These symptoms, often dismissed as normal aging or psychological issues, are deeply rooted in the physiological changes occurring within the brain.
The Neurobiological Underpinnings of Menopausal Symptoms
The exact mechanisms driving these cognitive and emotional symptoms are complex, involving a interplay of fluctuating hormone levels, typical age-related changes in brain structure and function, and the cumulative impact of life stressors. Estrogen, in particular, plays a crucial role in brain health, influencing neurotransmitter production (like serotonin, dopamine, and norepinephrine), glucose metabolism, blood flow, and neuronal connectivity. Its decline can therefore have widespread effects on mood regulation, memory, and executive function.
Compounding these biological changes are the myriad life challenges often faced by women in their 40s and 50s. This period frequently coincides with peak career responsibilities, the demands of parenting teenagers, caring for aging parents, navigating relationship changes, and significant financial pressures. These external stressors can deplete cognitive reserves, making women more susceptible to the impact of hormonal fluctuations.
However, a lesser-known yet increasingly recognized trigger for cognitive and emotional distress during menopause is the vasomotor symptom, commonly known as hot flashes and night sweats. These are far more than mere inconveniences or sources of embarrassment; a growing body of research indicates they can significantly impact brain health.
Vasomotor Symptoms: More Than Just a Flash of Heat
Hot flashes, occurring during the day, and night sweats, their nocturnal counterparts, are classified as vasomotor symptoms due to their effect on blood vessel constriction and dilation. During a hot flash, there’s a surge in norepinephrine and cortisol, leading to blood vessel dilation, increased blood pressure and heart rate, and sensations of warmth, flushing, and sweating. While the precise cause remains under investigation, one prominent theory points to falling estrogen levels affecting the hypothalamus, the brain’s thermostat, causing it to misregulate body temperature.
For years, these symptoms were considered benign, but emerging research paints a different picture. Vasomotor symptoms are increasingly viewed as a treatable medical condition due to their potential impact on blood vessels and the brain. One significant study involving 226 women, who wore monitors to track hot flashes and underwent MRI scans, revealed a correlation between frequent hot flashes and an abundance of "whole-brain white matter intensities." These patchy areas, once attributed solely to aging, are now considered predictive of future cognitive decline, increasing the risk of dementia twofold and stroke threefold.
The connection is thought to stem from changes in the cerebral blood vessels. A three-year study of 492 women demonstrated that those experiencing frequent hot flashes also exhibited unhealthy changes in their blood vessels, such as impaired ability to dilate. Other research has linked frequent hot flashes with increased markers of cardiovascular risk, including C-reactive protein (an inflammatory marker), insulin resistance, triglycerides, and lower HDL cholesterol. These vascular changes can compromise blood flow to the brain, contributing to cognitive impairment.

The Critical Role of Sleep Disruption
Beyond direct vascular effects, frequent hot flashes, particularly night sweats, profoundly disturb sleep. Many women may not even realize hot flashes are the culprit behind their insomnia, attributing their awakenings to general sleep disorders. This is because the intense heat sensation of a night sweat can dissipate by the time the surge in cortisol and norepinephrine jolts them awake, leaving them to wonder why they are repeatedly waking without a clear cause.
Chronic sleep deprivation, even if perceived as idiopathic insomnia, has devastating effects on brain function. It interferes with the brain’s ability to consolidate memories, metabolize toxins via the glymphatic system, and efficiently store daily information. This can lead to reduced connectivity in the hippocampus, a brain region vital for learning and memory. Furthermore, sleep loss makes the amygdala, the brain’s emotional center, more reactive, amplifying feelings of stress, anxiety, irritability, and frustration. These detrimental brain changes can manifest within days of inadequate sleep, making the cumulative impact of years of disrupted sleep during perimenopause and menopause profoundly significant.
Navigating the Healthcare Labyrinth: Advocacy and Education
The difficulty in obtaining appropriate care for menopausal symptoms is multi-faceted. Standard diagnostic tools for depression, such as the Patient Health Questionnaire (PHQ-9), contain several symptoms that overlap significantly with menopause-related sleep deprivation, including fatigue, trouble concentrating, and changes in appetite or sleep. This overlap can easily lead to a misdiagnosis of depression, diverting attention from the true hormonal imbalance.
A more systemic issue lies in the lack of comprehensive menopause-specific training within medical education. Surveys reveal that a significant majority of medical residents, including those in obstetrics and gynecology, feel inadequately prepared to discuss menopause with patients. This educational deficit contributes directly to healthcare professionals’ failure to inquire about hot flashes or sleep disturbances when women present with cognitive and emotional complaints.
Moreover, even when vasomotor symptoms are clearly linked to cognitive and emotional distress, many healthcare providers remain hesitant to prescribe menopausal hormone therapy (MHT), also known as hormone replacement therapy (HRT). This reluctance often stems from a practice of "defensive medicine," driven by concerns about litigation and a lingering misinterpretation of older research. Dr. Jerrold H. Weinberg, a Michigan-based menopause-trained gynecologist, highlights this reflex, noting that doctors often prioritize avoiding lawsuits when recommending treatments.
Re-evaluating Hormone Therapy: A Modern Perspective
The historical apprehension surrounding MHT largely originated from research conducted decades ago, which suggested an increased risk of breast cancer and stroke with certain types of hormones. However, more recent and nuanced research has refined this understanding. It is now understood that the risk profile of MHT is highly dependent on several factors, including the woman’s age, the specific type and dose of hormonal preparation, and the duration of use.
Current medical consensus, supported by organizations like The Menopause Society, indicates that for women under 60 and within 10 years of becoming postmenopausal, the benefits of MHT often outweigh the risks, particularly for those experiencing moderate to severe menopausal symptoms. Beyond symptom relief, MHT offers additional health benefits, such as a reduced risk of Alzheimer’s disease and osteoporosis. Dr. Weinberg emphasizes that for most women, these health benefits significantly counterbalance any potential risks. While antidepressants can alleviate some menopausal symptoms like mood disturbances and hot flashes, they come with their own side effect profiles and do not address the underlying hormonal deficiency, often making MHT a more targeted and effective treatment for menopause-specific issues.
Empowering Health Advocacy and Holistic Strategies
Given the complexities of diagnosis and treatment, women must become proactive advocates for their health. Seeking care from a menopause-trained health professional, easily identifiable through certifications from organizations like The Menopause Society, is paramount. Documenting symptoms meticulously, including their frequency, severity, and specific impact on daily life, provides invaluable data for clinicians. Being specific – detailing, for example, the exact number of nightly awakenings rather than a general complaint of "not sleeping well" – can lead to more accurate diagnoses and tailored treatment plans. Engaging in "shared decision-making" with healthcare providers, involving frank discussions about the pros and cons of various treatments, can empower patients and help shift clinicians away from a defensive mindset.
Beyond medical interventions, a holistic approach incorporating specific lifestyle strategies can significantly improve mental and emotional well-being during menopause.
- Fundamental Health Strategies: Prioritizing nutrition, physical activity, stress management, quality sleep, social connection, and a sense of purpose remains crucial. These foundational elements become even more vital as the body undergoes significant hormonal shifts. Regular self-assessment of these areas can identify neglected aspects.
- Experiment with Creatine: Beyond its known benefits for muscle and bone health, creatine may support mood, brain function, and reduce mental fatigue, even counteracting some negative effects of sleep deprivation. A daily dose of 5-7 grams of creatine monohydrate is often recommended.
- Regular Light Exposure: Morning and late afternoon sunlight exposure helps regulate the body’s circadian rhythm, promoting alertness during the day and better sleep at night. Studies show morning outdoor time correlates with quicker sleep onset, longer sleep duration, and fewer awakenings.
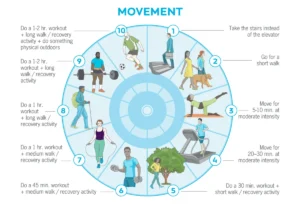
- Moderate Exercise: While intense workouts can be counterproductive due to increased injury risk and longer recovery times in middle age, short bursts of moderate exercise can boost alertness. Gentle activities like yoga or stretching can aid relaxation before bed. Tuning into the body’s signals, especially after poor sleep, and adjusting intensity (e.g., opting for Zone 2 cardio or reducing resistance training volume) is key.
- Cognitive Behavioral Therapy for Insomnia (CBT-I): This evidence-based therapy equips individuals with skills and cognitive reframes to improve sleep quality, such as maintaining a consistent wake-up time regardless of prior night’s sleep.
- Realistic Stress Management: Re-evaluating responsibilities and commitments is essential. Tracking time and bandwidth can reveal areas for downsizing or delegating. Identifying specific sources of stress allows for targeted resolution, empowering women to say "no" more often to protect their mental and emotional capacity.
- Cooling Technology: Optimizing the sleep environment with lower thermostat settings, fans, or electric cooling mattress pads can reduce night sweats and improve sleep quality.
- Frequent Breaks: During periods of brain fog, short breaks (20 minutes of complete rest, a 5-minute mind-body scan) can help reset cognitive function. Observing physical sensations and thoughts without judgment can provide clarity and a sense of refreshment.
- Circulation-Promoting Diet: Adopting dietary patterns like the MIND or Mediterranean diets, rich in vegetables, fruits, whole grains, and healthy fats, supports both cardiovascular and cerebrovascular health, reducing the risk of cognitive decline and depression. Nitrate-rich foods like beets and leafy greens can temporarily improve brain blood flow and memory.
The Transformative Potential of Menopause
While the challenges of menopause can be profoundly frustrating, this life stage also presents a unique opportunity for introspection and re-evaluation. The forced slowdown and cognitive shifts can compel women to critically assess their priorities, asking fundamental questions about how they allocate their finite mental and physical resources. This period can become a catalyst for simplifying life, delegating tasks, and learning to say "no" without guilt, thereby creating space for what truly matters: cherished relationships, personal well-being, and pursuing activities that bring genuine joy and purpose.
For many, regaining clarity and energy through appropriate medical intervention and lifestyle adjustments leads not to a return to previous patterns of overcommitment, but to a conscious choice to embrace a more balanced and fulfilling life. The experience of navigating menopause, with all its complexities, can ultimately empower women to redefine success, prioritize self-care, and live more authentically, recognizing the profound interplay between hormonal health, cognitive function, and overall well-being.
References
[The original article’s references would be listed here, as indicated by the "Click here to view the information sources referenced in this article." placeholder.]