The insidious onset of cognitive and emotional disturbances often mislabeled as depression can profoundly impact women approaching and experiencing menopause. For one individual, a common Friday night attempt to choose a restaurant became a stark illustration of a mind increasingly shrouded in a "pile of garbage." Simple proper nouns, once readily accessible, vanished into the "deep recesses of my brain," only to resurface hours later with a sudden, frustrating clarity – "Texas Roadhouse!" This wasn’t merely the typical "sludginess" often associated with middle age; it was a pervasive mental haziness that began to significantly impair daily function and professional productivity in her late 40s and early 50s. The struggle extended beyond forgotten names, manifesting as a profound inability to focus on work, read, or engage with the world with customary mental acuity. This personal account highlights a critical, yet often overlooked, dimension of the menopausal transition: its profound impact on cognitive and emotional well-being, frequently misattributed to other conditions.
The Personal Toll: A Journey Through Misdiagnosis
The individual’s experience illustrates a common, frustrating path for many women. Faced with debilitating brain fog, pervasive fatigue, and a striking lack of "gumption," she sought medical advice. Three healthcare professionals independently recommended antidepressants, a common first-line response to symptoms that mimic depression. However, each trial, including varying doses and different medications, only exacerbated her condition, leaving her feeling "even worse" or "like a zombie." A prescribed sleeping pill similarly failed, inducing a drugged state without alleviating the underlying issues. Further diagnostic tests for thyroid function and anemia yielded no answers. A two-year odyssey through a "revolving door of doctors" involved attempts with various supplements, "mushroom coffee," and products promising cognitive enhancement, all to no avail.
The turning point came during a routine annual gynecological exam. A casual mention of vaginal dryness prompted a series of questions from her gynecologist that diverged from typical gynecological concerns: sleep quality, mood, energy levels, hot flashes, and critically, brain fog. Her resigned, "Funny you should mention brain fog… I feel like I’m barely alive," resonated. By the end of that appointment, a profound realization dawned: the persistent symptoms were not depression, but rather a manifestation of menopause. Prescriptions for estradiol and progesterone quickly followed, leading to a dramatic improvement within days. The ability to think, write, follow conversations, and work beyond noon returned. Crucially, years of fragmented sleep were replaced by restorative rest, marking a complete reversal of her debilitating symptoms.
Understanding the Menopausal Transition: More Than Just a "Life Stage"
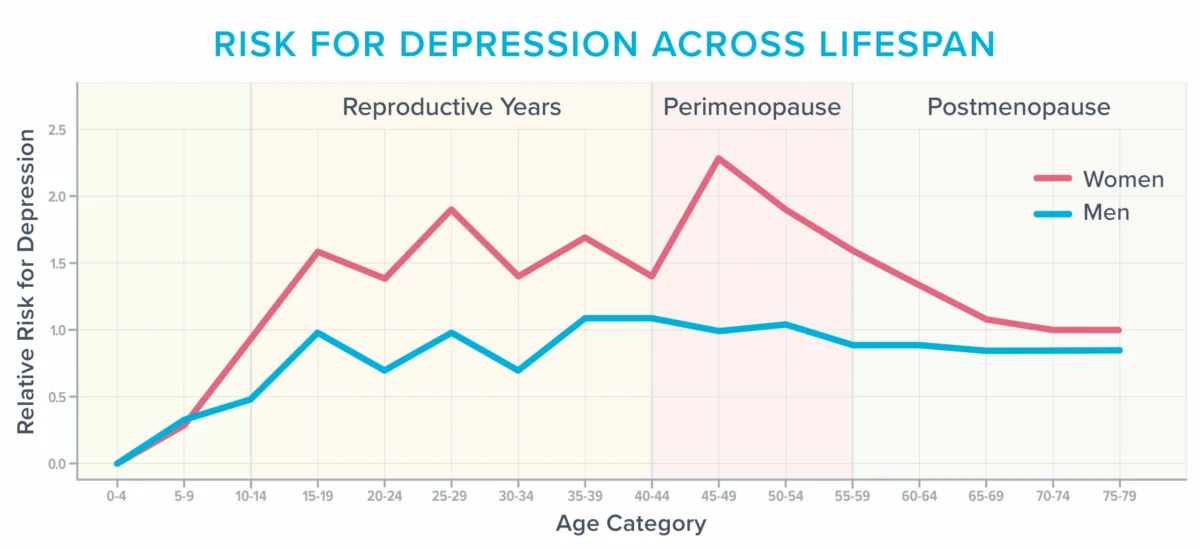
Menopause is not a medical condition or a disease; it is a significant biological transition in a woman’s life, akin to puberty. It is clinically defined as 12 consecutive months without a menstrual period, after which a woman is considered "postmenopausal." The period leading up to this, known as perimenopause, can last several years, characterized by fluctuating and ultimately declining levels of key hormones, primarily estrogen and progesterone. These hormonal shifts trigger a wide array of symptoms that can significantly impact quality of life. While weight gain and reduced sex drive often receive considerable attention, the American College of Obstetricians and Gynecologists (ACOG) reports that approximately 40% of women experience increased irritability, mood swings, anxiety, fatigue, and trouble concentrating during and after menopause. This period also represents a heightened vulnerability for developing depression, particularly for those with a history of the condition, as illustrated by data showing a peak in women’s depression risk around the perimenopausal years.
Beyond the direct hormonal influence, women in their 40s and 50s often contend with significant life stressors that can compound cognitive and emotional challenges. These include peak career responsibilities, caring for adolescent children or aging parents, adjusting to an empty nest, marital re-evaluation, and financial pressures related to education or healthcare. These external factors can undeniably "siphon cognitive capacity," yet a critical, often under-recognized, internal trigger for cognitive and emotional distress during menopause is the hallmark symptom itself: the hot flash.
The Anatomy of Vasomotor Symptoms and Their Neurological Impact
Hot flashes (daytime occurrences) and night sweats (nocturnal occurrences) are collectively known as vasomotor symptoms (VMS). These events involve the constriction and dilation of blood vessels, influencing blood pressure and sweating. During a hot flash, there is a surge in norepinephrine and cortisol, leading to blood vessel dilation, increased heart rate, and often a sensation of warmth spreading through the upper body, reddening of the skin, sweating, and sometimes palpitations, anxiety, or faintness. While the exact mechanism remains elusive, a leading theory suggests that falling estrogen levels disrupt the hypothalamus, the brain’s temperature-regulating center, leading to a dysregulation of the body’s internal thermostat.
For years, VMS were largely dismissed as mere inconveniences or sources of embarrassment. However, a growing body of research is fundamentally changing this perception, revealing that hot flashes and night sweats are more than just discomforting; they may have significant implications for cardiovascular and brain health. Consequently, an increasing number of experts now advocate for treating VMS as a medical condition rather than an unavoidable nuisance.
Research has unveiled concerning links between VMS and brain changes. One significant study involving 226 women utilized monitors to track hot flashes and Magnetic Resonance Imaging (MRI) to examine brain structure. Women experiencing the most frequent hot flashes exhibited a higher prevalence of "whole-brain white matter intensities" – patchy areas once thought to be a benign consequence of aging, but now recognized as a predictor of future cognitive decline. Individuals with an abundance of these lesions face double the risk of dementia and triple the risk of future stroke, underscoring the severity of this connection.
The mechanism linking hot flashes to these brain lesions appears to involve changes in the brain’s delicate vascular system. A three-year study of 492 women demonstrated that frequent hot flashes correlated with unhealthy alterations in blood vessels, specifically a reduced ability to dilate in response to increased blood flow. This impaired vascular function can compromise the delivery of oxygen and nutrients to brain tissue. Further research has associated frequent hot flashes with increased markers of inflammation, oxidative stress, and endothelial dysfunction, all of which contribute to vascular damage and heightened risk for cardiovascular disease and neurodegenerative conditions.
The Crucial Role of Sleep Disruption
Beyond direct vascular effects, frequent hot flashes profoundly impact the brain through chronic sleep disturbance. Many women, like the individual in the opening narrative, do not consciously attribute their awakenings to night sweats. The surge of cortisol and norepinephrine that jolts them awake may dissipate before the heat sensation becomes noticeable, leading to the perception of unexplained insomnia or sleep apnea. These repeated, unremembered awakenings severely disrupt the brain’s ability to consolidate memories, metabolize toxins accumulated during the day, and efficiently store new information. This chronic sleep deprivation can lead to lost connectivity in the hippocampus, a brain region vital for learning and memory. Furthermore, insufficient sleep heightens the reactivity of the amygdala, the brain’s emotional center, making individuals more prone to stress, anxiety, irritability, and anger. These detrimental brain changes can manifest after just days of disrupted sleep, illustrating the profound cumulative effect of years of menopausal sleep disturbance.
The Diagnostic Labyrinth: Why Help Can Be Elusive
The diagnostic process itself often contributes to the misattribution of menopausal symptoms to depression. Healthcare professionals commonly use tools like the Patient Health Questionnaire (PHQ-9) depression scale. A score indicating four or more symptoms often leads to a depression diagnosis. However, a critical overlap exists: four symptoms on the PHQ-9 checklist directly correspond with symptoms of menopause-related sleep deprivation: trouble falling/staying asleep, feeling tired or having little energy, changes in appetite or weight, and trouble concentrating. A woman battling persistent night sweats and resulting sleep loss might tick these boxes, leading to an antidepressant prescription when the root cause is hormonal.
A significant systemic issue exacerbating this problem is the pervasive lack of menopause-specific training within the medical community. Surveys reveal that 80% of medical residents feel "barely comfortable" discussing menopause, and remarkably few residency programs, including those for obstetrics and gynecology, offer comprehensive training in menopausal care. This educational gap explains why many healthcare professionals fail to inquire about hot flashes or sleep disturbances when patients present with fatigue, lack of motivation, and cognitive difficulties.
Even when VMS are clearly linked to cognitive and emotional symptoms, many clinicians hesitate to prescribe Menopausal Hormone Therapy (MHT), also known as Hormone Replacement Therapy (HRT). This reluctance often stems from a practice of "defensive medicine," where concerns about potential litigation outweigh the consideration of patient benefit. Dr. Jerrold H. Weinberg, a Michigan-based menopause-trained gynecologist, notes that the fear of being sued is a primary reflex when recommending treatments.
Demystifying Hormone Therapy: What the Research Actually Says

The apprehension surrounding MHT largely originates from research conducted decades ago, particularly the Women’s Health Initiative (WHI) study, which linked certain types of hormones to a slightly increased risk of breast cancer and stroke. However, more recent and nuanced research has refined this understanding. It is now recognized that the magnitude of these risks is influenced by several factors, including a woman’s age, the specific dose and type of hormonal preparation, and the duration of use.
Current consensus among many experts indicates that for women under 60 or those who have been postmenopausal for fewer than 10 years, the benefits of MHT often outweigh the risks, particularly for moderate to severe menopausal symptoms. Furthermore, MHT can offer significant health benefits, such as a reduced risk of developing Alzheimer’s disease and osteoporosis. Dr. Weinberg emphasizes that for most women, the health benefits of MHT substantially outweigh the risks. Despite this, some healthcare professionals still opt for antidepressants to manage mood, sleep, and hot flashes, often perceiving them as a "safer bet" due to defensive medicine practices, despite antidepressants having their own set of side effects.
Empowering Advocacy: Taking Control of Your Menopausal Health
Navigating the complexities of menopausal health requires informed self-advocacy. Dr. Weinberg and Helen Kollias, PhD, a physiology and molecular biology expert and science advisor at Precision Nutrition, offer crucial advice:
- Seek Menopause-Trained Professionals: Look for healthcare providers who explicitly list menopause as a focus area in their biographies or who hold certifications from reputable organizations like the Menopause Society (formerly NAMS). A database of certified practitioners is often available through these organizations.
- Document Your Symptoms Meticulously: Keep a detailed log of your symptoms, including their nature, frequency, severity, and any triggers or alleviating factors. This written record serves as a valuable resource during appointments, especially if brain fog or anxiety makes it difficult to recall details. Track hot flashes/night sweats, sleep quality (awakenings, duration), mood changes (irritability, anxiety, sadness), energy levels, and cognitive function (memory, focus).
- Be Specific in Your Communication: Vague statements like "I don’t sleep well" are less effective than precise descriptions. For example, "During the past seven days, I’ve only achieved four uninterrupted hours of sleep once. I wake, on average, five times a night, and my longest stretch of sleep is typically three hours." If you use a smartwatch or other health trackers, be prepared to share the data.
- Engage in Shared Decision-Making: This medical concept involves a frank discussion between patient and clinician about the benefits and risks of a proposed treatment, leading to a collaborative decision. Encourage this approach by asking pointed questions such as: "What are the specific benefits of this treatment for my symptoms?"; "What are the potential side effects or risks, both short-term and long-term?"; "Are there alternative treatments, and what are their pros and cons?"; and "How will we monitor the effectiveness and safety of this treatment?" This active participation can help shift a clinician away from a purely "defensive medicine" mindset.
Holistic Strategies for Mental and Emotional Well-being During Menopause
Beyond medical interventions, lifestyle adjustments play a crucial role in managing menopausal cognitive and emotional symptoms. While there’s no "special diet" for VMS beyond avoiding known triggers like caffeine, alcohol, and spicy foods (and studies show soy products are not as effective as once thought for VMS), fundamental health strategies are paramount.
-
Prioritize Fundamental Health Strategies: Re-evaluate and strengthen foundational habits:
- Nutrition: Are you consuming a balanced, whole-foods diet?
- Physical Activity: Are you consistently engaging in movement you enjoy?
- Stress Management: Do you have effective strategies to cope with daily stressors?
- Sleep Hygiene: Are you prioritizing consistent, quality sleep?
- Social Connectedness: Are you nurturing meaningful relationships?
- Sense of Purpose: Do you have activities that provide meaning and fulfillment?
Addressing barriers to these fundamentals is critical.
-
Experiment with Creatine: This supplement, known for its benefits in muscle and bone health, may also improve mood, enhance brain function, reduce mental fatigue, and counteract some negative effects of sleep deprivation. A daily dose of 5-7 grams of creatine monohydrate is often recommended.
-
Regular Light Exposure: Morning and late afternoon sunlight exposure helps regulate the body’s internal clock (circadian rhythm), promoting alertness during the day and better sleep at night. Studies show that morning light exposure can lead to faster sleep onset, longer sleep duration, and fewer awakenings. Sunlight also has a positive impact on mood and concentration.
-
Adjust Exercise Intensity: While exercise is vital, overly intense or long sessions can exacerbate fatigue and irritability during menopause, especially with impaired recovery. Injuries are also more common. Short bursts of movement, like a 5-10 minute walk or quick bodyweight exercises, can provide an "alert refresh" during the day. Gentle exercises like yoga or stretching can aid relaxation before bed, but avoid intense activity too close to bedtime. The key is to listen to your body and adjust workout intensity and volume based on sleep quality and recovery, opting for moderate sessions (e.g., Zone 2 cardio) or reduced sets/reps when feeling depleted.
-
Investigate Cognitive Behavioral Therapy for Insomnia (CBT-I): This evidence-based therapy equips individuals with skills and mental reframes to improve sleep quality. Techniques include maintaining a consistent wake-up time regardless of prior night’s sleep and addressing maladaptive thoughts about sleep.
-
Get Real About Stress: Menopause can be a time of re-evaluation. Critically assess your responsibilities and commitments. Track how you spend your time and mental energy, then identify areas for reduction or delegation. Ask: "What am I doing that I no longer enjoy or find necessary?"; "What can I delegate or simplify?"; "Where can I set better boundaries?" Tools like the "Wheel of Stress Assessment" can help pinpoint specific stressors. Learning to say "no" more often can free up vital bandwidth for self-care.
-
Experiment with Cooling Technology: A cooler sleep environment can significantly reduce night sweats and improve sleep quality. This can involve lowering the thermostat, using a fan, or investing in specialized cooling mattress pads.
-
Take Frequent Breaks: When brain fog descends, productivity inevitably wanes. Implement intentional breaks throughout the day. This could involve stepping away from your desk to stretch, gaze out a window, listen to music, or simply sit quietly for 20 minutes. A quick 5-minute mind-body scan – lying comfortably, closing your eyes, and observing physical sensations and thoughts without judgment – can offer a rapid refresh.
-
Adopt a Circulation-Promoting Diet: The same dietary patterns that protect heart health also benefit brain health. Diets like the MIND (Mediterranean-DASH Intervention for Neurodegenerative Delay) and Mediterranean diets, rich in vegetables, fruits, whole grains, healthy fats (olives, fish), and legumes, are associated with a reduced risk of Alzheimer’s disease and depression. Additionally, nitrate-rich foods such as beets and dark leafy greens may temporarily improve memory and cognitive function by promoting blood vessel dilation and increasing blood flow to the brain.
The Upside: A Call for Reassessment and Prioritization
While the challenges of menopausal cognitive and emotional symptoms can be profoundly frustrating, this life stage also presents a unique opportunity for introspection and re-evaluation. For the individual who experienced debilitating brain fog, the diminished capacity forced an existential question: "Do I really need to be doing this?" This query extended beyond career, prompting a reassessment of how to allocate finite mental resources. The realization that working eight hours a day wasn’t a mandatory necessity, that meal preparation could be simplified, and that saying "no" more often could free up capacity for truly meaningful pursuits transformed her outlook. Prioritizing visits with aging parents, answering a child’s call from college, or enjoying a leisurely walk with a friend became paramount.
With the aid of appropriate hormonal therapy and intentional lifestyle adjustments, energy and mental clarity returned. However, the habit of ending the workday earlier persisted, not out of necessity, but out of choice. Menopause, therefore, can become a catalyst for profound personal recalibration, allowing women to reclaim agency over their time and energy, and to consciously prioritize what truly matters, fostering a more balanced and fulfilling postmenopausal life.
References
Click here to view the information sources referenced in this article.